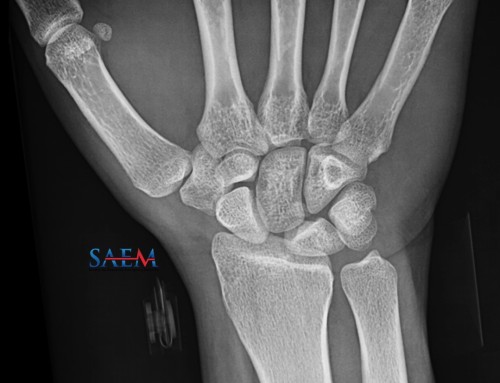
An 82-year-old woman presents with left hip pain after a mechanical fall while cleaning the kitchen floor. When EMS arrived, the left leg was foreshortened and externally rotated. The paramedics administered 10 mg of IV morphine, but she is still writhing in pain on arrival. The AP pelvic x-ray demonstrates a left femoral neck fracture (arrow). You consider performing a fascia iliaca nerve block for better pain control.
Why do a fascia iliaca nerve block?
Multiple studies have shown decreased in-hospital mortality and complications when regional anesthesia is performed. Specifically for hip fractures, fascia iliaca blocks led to a reduction of postoperative complications from 33% to 20%1 along with decreased mortality, deep vein thromboses, altered mental status, and pulmonary complications.2
Goal of the fascia iliaca nerve block
The goal of this nerve block is to maximize analgesia, while minimizing side effects such as respiratory depression, delirium, hypotension, and nausea/vomiting that may be associated with IV opioid administration. The target of the anesthetic injection is the potential space between the iliacus muscle and the fascia that overlies it (fascia iliaca), within which the femoral nerve and lateral femoral cutaneous nerve (LFCN) course. A large volume injection (40 mL) will lead to appropriate fascial spread and anesthesia of the femoral nerve (88%), LFCN (90%), and sometimes the obturator nerve.3

Figure 1. Anesthetic distribution of the fascia iliaca block (Source: NYSORA.com)
When should I not perform the fascia iliaca block (contraindications)?
- Any anticoagulation, besides aspirin and NSAIDs
- Overlying cellulitis at the skin puncture site
- Ipsilateral fractures at high risk of compartment syndrome, such as tibial plateau fractures
Equipment

Figure 2. A layout of the equipment needed for a fascia iliaca nerve block
The necessary equipment for this nerve block includes the following:
Sterile precautions
- Sterile ultrasound probe cover
- Sterile gloves
- ChloraPrep wipe
Identifying the anatomy
- Bedside ultrasound with a linear transducer
Instilling the anesthetic
- Lidocaine 1% (2-5 mL) for local wheal of anesthetic
- Local long-acting anesthetic (e.g., 40 mL of 0.2% ropivacaine) for nerve block
- Sterile saline flush
- 10 mL syringe
- 60 mL syringe
- Extension tubing
- 18-gauge needle
- 25-gauge needle
- 21-gauge nerve block needle

Figure 3. Syringe and nerve block needle set-up for administration of anesthetic agent
Anesthetic medication options
For a longer period of regional anesthesia, we recommend ropivacaine or bupivacaine. Given the higher cardiac toxicity of bupivacaine due it’s highly lipophilic nature compared to other local anesthetics, we suggest 40 mL of 0.2% ropivacaine as the first-line agent.4,5 Lidocaine is not preferred given it’s shorter duration of action, which is contradictory to the goal of prolonged analgesia.
| Local anesthetic agent | Relative potency | Duration of action | Maximum allowable subcutaneous dose (mg/kg) |
|---|---|---|---|
| Bupivacaine | High | Long | 2 |
| Etidocaine | High | Long | 4 |
| Lidocaine | Low | Medium | 4.5 |
| Mepivacaine | Intermediate | Medium | 4.5 |
| Prilocaine | Intermediate | Medium | 8 |
| Ropivacaine | Intermediate | Long | 3 |
Figure 4. Local amide-based anesthetic agents and their pharmacokinetic effects, adapted from Goldfrank’s Toxicologic Emergencies6
Technique
Equipment positioning
Start by setting up an equipment stand on the same side of the bed as the patient’s fracture, with the ultrasound machine on the contralateral side of the fracture. You will stand on the side of the fracture facing towards the head of the bed and looking across the patient’s body at the ultrasound machine.
Sterile preparation
- Wipe the ipsilateral inguinal area with the ChloraPrep and drape the area.
- Fill the 60 mL syringe with 4 mL of 0.2% ropivacaine.
- Attach the syringe to the extension tubing and nerve block needle.
- Remove air from the tubing and “prime it” with the ropivacaine from the syringe.
- Place the sterile ultrasound probe cover on the probe.
Anatomy identification
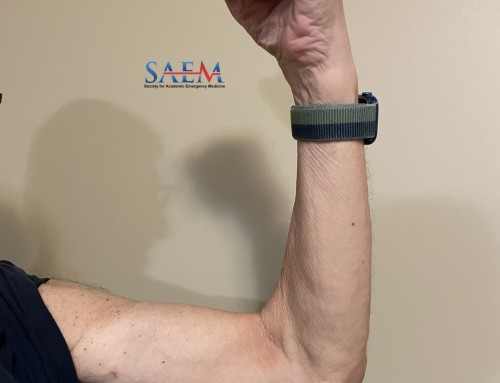
- Position the linear, high-frequency ultrasound probe held in horizontal orientation with the probe marker pointed towards the patient’s right side (Figure 5).

Figure 5. A patient’s left anterior leg with the patient’s head located towards the top at the photo. The ultrasound’s linear probe is positioned horizontally at the level of the common femoral artery and vein. (Source: NYSORA.com)
- Locate the femoral vessels ideally at the level of the common femoral artery and vein.
- Slide the probe laterally until you see the iliacus and sartorius muscles (Video 1). The iliacus muscle will be in the same plane as the femoral vessels, and the sartorius will be superior and lateral (Figure 6).

Video 1 and Figure 6. Ultrasound image showing how the femoral vessels can be used to guide the identification of the iliacus muscle, fascia iliaca, and sartorius muscle in a patient’s left hip. In these images, medial is towards the left of the screen and lateral is towards the right.
Instillation of anesthetic agent
- Using a 10 mL syringe and 25 gauge needle, deposit a small wheal of local anesthetic (e.g. lidocaine) directly adjacent to the lateral surface of the ultrasound probe.
- Switch to the longer 21 gauge nerve block needle, which is affixed to an extension tubing and 60 mL ropivacaine-filled syringe (Figure 3). The primary operator should be sterilely gowned and hold the nerve block needle, while a secondary operator should hold the ropivacaine syringe, being in charge of instilling the anesthetic when needed.
- Primary operator: Insert the nerve block needle at a steep 45-60 degree angle through the wheal and advance in a plane through the subcutaneous tissue until you visualize the tip of the needle underneath the fascia iliaca. You will likely feel pop or change in resistance as you pass through the fascia iliaca.
- Secondary operator: Once the needle is appropriately positioned by the primary operator, inject a micro-aliquot of anesthetic (0.5 to 1 mL) to see if the fascia iliaca appropriately dissects off the iliacus muscle (Video 2).
- If the needle tip is placed inappropriately above (superficial to) the fascia iliaca in the subcutaneous tissue or within the iliacus muscle, make in-plane adjustments of the needle tip and instill additional micro-aliquots until appropriate localization.
- Once the needle is appropriately positioned, inject the entire volume of the 40 mL 0.2% ropivacaine. Clear the ropivacaine remaining in the extension tubing with a few mL’s of the sterile saline flush after swapping the 60 mL syringe with a sterile saline flush.
- Adequate anesthesia can take up to 30-60 minutes as the ropivacaine tracks upwards into the pelvis.
Alternative Technique
A suprainguinal approach may lead to more proximal spread of anesthetic and more successful pain control; however, the approach relies on adequate visualization of the patient’s internal oblique muscle, which is often tiny and hard to see in the elderly. The suprainguinal approach mirrors the above approach to identify the iliacus muscle. Then slide the probe superiorly along the iliacus muscle until the probe is above the inguinal canal. Then rotate the probe marker 90 degrees so that it points towards the umbilicus. The sartorius and internal oblique muscles will form a “bowtie” shape with the iliacus muscle below them. Inject the anesthetic in between the bowtie, aiming just below the fascia iliaca as described in the traditional approach (Figure 8).

Figure 8. Suprainguinal fascia iliaca injection site for a patient’s hip from a sagittal view. The left is towards the hip, and the right is towards the umbilicus. Note that the sartorius and internal oblique muscles form a “bowtie” configuration. (Source: NYSORA.com)

Want to learn more?
Join Dr. Shyy and other UCSF expert ultrasound educators at the High Risk Hawaii Conference in Maui April 14-18, 2019, where they will teach hands-on ultrasound-guided nerve blocks, vascular access, and orthopaedic procedures. Dr. Amal Mattu will also be there to lecture and teach an Advanced EKG Bootcamp!
References
- Pedersen S, Borgbjerg F, Schousboe B, et al. A comprehensive hip fracture program reduces complication rates and mortality. J Am Geriatr Soc. 2008;56(10):1831-1838. https://www.ncbi.nlm.nih.gov/pubmed/19054201.
- Luger T, Kammerlander C, Gosch M, et al. Neuroaxial versus general anaesthesia in geriatric patients for hip fracture surgery: does it matter? Osteoporos Int. 2010;21(Suppl 4):S555-72. https://www.ncbi.nlm.nih.gov/pubmed/21057995.
- Capdevila X, Biboulet P, Bouregba M, Barthelet Y, Rubenovitch J, d’Athis F. Comparison of the three-in-one and fascia iliaca compartment blocks in adults: clinical and radiographic analysis. Anesth Analg. 1998;86(5):1039-1044. https://www.ncbi.nlm.nih.gov/pubmed/9585293.
- Feldman H, Arthur G, Covino B. Comparative systemic toxicity of convulsant and supraconvulsant doses of intravenous ropivacaine, bupivacaine, and lidocaine in the conscious dog. Anesth Analg. 1989;69(6):794-801. https://www.ncbi.nlm.nih.gov/pubmed/2511782.
- Reiz S, Nath S. Cardiotoxicity of local anaesthetic agents. Br J Anaesth. 1986;58(7):736-746. https://www.ncbi.nlm.nih.gov/pubmed/2425836.
- Kaufman R. Local Anesthetics. In: Goldfrank L, ed. Goldfrank’s Toxicologic Emergencies. New York, NY: McGraw-Hill; 2011:967.