Case Writer: Clare Desmond, MD
Peer Reviewer and Editor: Nikita Joshi, MD
Keywords: Cardiac arrest, Perimortem C-section
Educational Objectives
Medical:
- Recognize and manage cardiac arrest in pregnant patients
- Identify need for perimortem CS
- Perform perimortem CS
Communication:
- Communicate emergent need for perimortm CS to team leader
- Consult NICU and OB stat
Case Synopsis
28 year old female, 37 weeks pregnant, BIBEMS after high speed MVC. Pt was a restrained driver in a head-on collision with a tree. Estimated speed at impact was 75 mph. The car was completely damaged with spider webbing of the windshield. Pt was responsive to pain but was not oriented in the field. EMS noted a protuberant abdomen. Upon arrival in the ED, her initial GCS was 5 (abnormal flexion to pain with decorticate response), it is noted that the pt becomes pulseless within 5 minutes of arrival to the ED and has an asystolic cardiac arrest.
- Initiate ATLS on high speed MVC pt
- Initiate ACLS on asystolic cardiac arrest
- Identify pregnant pt with uterine fundus greater than 20 cm above pubic symphysis
- Initiate and complete perimortem CS within 5 minutes loss of pulses
Learners
- ED residents
- OB residents
- Pediatric residents
- Medical students
- ED nurses
- Nursing students
Location:
ED resuscitation bay
Patient
28 yo female, 37 wks pregnant
Equipment
- Advanced airway equipment
- Airway adjuncts
- Bedside ultrasound
- Cardiac arrest code cart
- Cervical c-spine collar
- IV fluid
- Monitor
- Neonatal warmer
- Retractors
- pRBCs
- Scalpel – 10 blade
- Spinal immobilization back board
- Stretcher with sheets
Moulage
- Ecchymotic patches on chest
- Fetus manikin
- Gravid abdomen with uterus moulage capable of being cut
- Manikin for with trauma and pregnancy capabilities
Confederates
- EMS provider— helpful, gives initial history and discuss initial vitals on scene, gives details of completely destroyed car and tree at the scene of the accident
- Husband- frantic, informs team that pt is pregnant
- Nurse – helpful, performs orders given by team, gives helpful hints suggesting decision to perform CS
- NICU (voice) – calls when consulted, discusses case
- OB (voice) – calls when consulted, not in house, discusses case
Supporting Files / Media
- Asystole rhythm strip
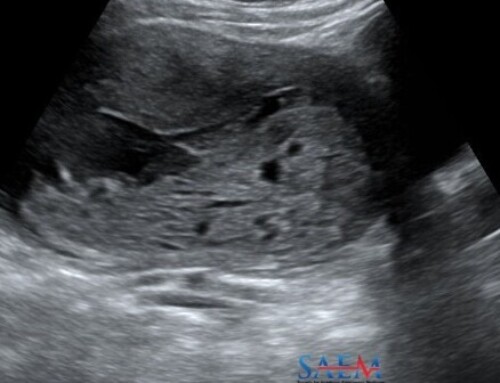
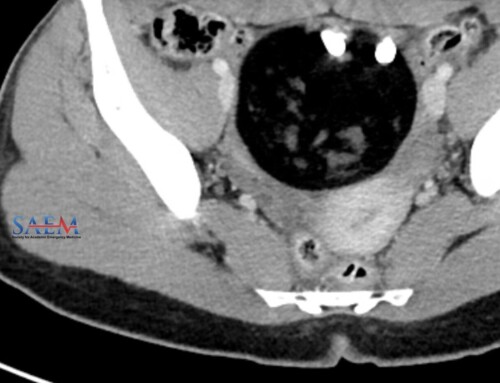
- Bedside ultrasound trans-abdominal images of large fetus with fetal heart movement
- Labs: Shock panel, Urine HCG, Type and Screen / Cross
Translation | |
Abd | abdominal / abdomen |
BIBEMS | brought in by EMS |
BP | blood pressure |
CS | cesarean section |
HR | heart rate |
IV | intravenous |
MVC | motor vehicle collision |
Neg | negative |
RR | respiratory rate |
PEA | pulseless electrical activity |
pRBCs | packed red blood cells |
TA | transabdominal |
T | temperature |
US | ultrasound |
References used:
- Newfield E. Third-Trimester Pregnancy Complications. Prim Case Clin Office Pract. Elsevier 39 (2012). 95-113.