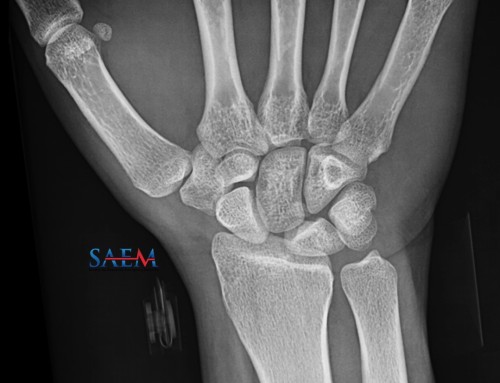
A 22 year-old male was playing football when he fell, landing on his outstretched left arm with his thumb flexed. He now has pain at the base of his thumb. This AP view of the hand best demonstrates the injury (photo credit).
What is this fracture, what additional imaging is needed, and what should be the management plan?
First Metacarpal Fractures [1, 2]
Mechanism
- Fall on hand with thumb in flexion and axial loading of the first metacarpal
Physical Exam
- Tenderness to palpation of the first metacarpal
- Swelling over the radial aspect of the hand
Classifications (Figure 1)
- Extraarticular
- Intraarticular
- Bennett Fracture: A partial intra-articular fracture at the base of the 1st metacarpal with a single fracture fragment displaced to the medial and palmar aspect of the bone
- Rolando Fracture:– A complete and comminuted intraarticular fracture, usually in a T or Y shape

(Original images used with permission from Dr. Jeffrey Daniels)
Management
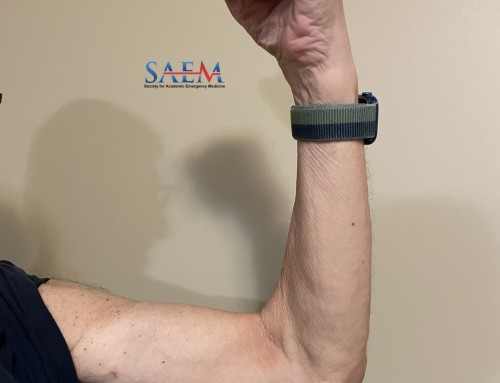
- Thumb spica splint with IP joint in extension (Figure 2)
- Extraarticular
- Up to 20-30 degrees of angulation may be tolerated and managed conservatively
- Outpatient follow-up with hand surgery within 1 week (sooner if severely angulated)
- Intraarticular
- Urgent (≤3 days) follow-up with hand surgery clinic for likely operative fixation
- As always, call an orthopedist emergently, if there is an open fracture or neurovascular compromise

(Illustrated by Dr. Tabitha Ford)
For more cases like these, you can subscribe to the Ortho EM Pearls email series hosted by Drs. Will Denq, Tabitha Ford, and Megan French, who have kindly shared some of their content with ALiEM.
References
- Mailhot T, Lyn E. Hand. In: Marx J, ed. Rosen’s Emergency Medicine Concepts and Clinical Practice. 8th ed. Philadelphia, PA: Elsevier, Saunders; 2014: 534-569.e2
- Diaz-Garcia R, Waljee J. Current management of metacarpal fractures. Hand Clin. 2013;29(4): 507-518. doi: 10.1016/j.hcl.2013.09.004.