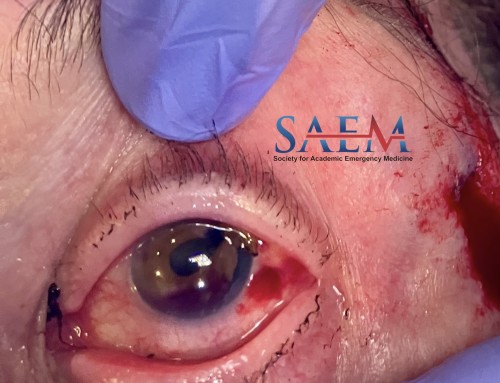
A 54 year-old male presents to the emergency department with an eye complaint. The patient works as a cook and while cleaning the grill several hours ago felt something fly into his eye. He did not immediately feel pain, but notes blurred vision and an increasing pressure-like sensation in his left eye. He describes his left-sided blurred vision as a haziness, like cobwebs over his eye. He has been able to open his eye and keep it open without difficulty.
A 54 year-old male presents to the emergency department with an eye complaint. The patient works as a cook and while cleaning the grill several hours ago felt something fly into his eye. He did not immediately feel pain, but notes blurred vision and an increasing pressure-like sensation in his left eye. He describes his left-sided blurred vision as a haziness, like cobwebs over his eye. He has been able to open his eye and keep it open without difficulty.
Physical Exam
- BP: 135/81
- HR: 83
- RR: 20
- Temp: 97.9F
- SpO2: 98%
- Vision: Pupils are equally round and reactive to light, extraocular movements are intact.
- Right eye: Visual acuity 20/20
- Left eye: Visual acuity 20/40, “hand motion” vision at 3 feet. No eyelid lacerations, bleeding, or discharge. intraocular pressure 15 mmHg
Differential Diagnoses
- Foreign body
- Corneal abrasion
- Corneal ulcer
- Retinal detachment
- Macular degeneration
- Vitreous detachment
- Vitreous hemorrhage
Available Equipment
- Ophthalmoscope
- Topical ophthalmic anesthetic (ie. proparacaine or tetracaine)
- Fluorescein strips
- The Wood’s lamp: A source of long wave ultraviolet light with a magnifying glass that can be used to detect fluorescein. Use with caution. Sensitivity may only be 50% in the detection of common corneal pathologies [1].
- The slit lamp: considered the gold standard in detection of corneal and anterior chamber pathologies. Intimidated? Check out @MRamzyDO’s helpful slit-lamp infographic.
- Point-of-care ultrasound (POCUS): noninvasive, can detect several ocular pathologies, as seen in the table below [2]:
| Pathology | POCUS sensitivity | POCUS specificity |
|---|---|---|
| Retinal Detachment | 96.9% | 88.1% |
| Vitreous Hemorrhage | 81.9% | 82.3% |
| Vitreous detachment | 42.5% | 96% |
Ocular Physical Examination
A Wood’s lamp examination of this patient showed normal fluorescein uptake. There was no corneal abrasion visualized. Both the upper and lower eyelids were flipped and showed no foreign body. Slit lamp findings showed a clear cornea.
Following application of a tegaderm to the affected eye and a generous amount of gel, the below images were obtained using a linear probe set to the greatest amount of gain:

Figure 1: Ocular ultrasound depicting debris in the posterior eye

Figure 2: Ocular ultrasound showing another area of debris in the posterior eye
Discussion
The ultrasounds above demonstrate classic findings for vitreous hemorrhage, in which the posterior chamber contains materials of varying echogenicity [2]. The vitreous humor is an avascular gel-like substance that occupies the space between the lens and the retina in the eye. Vitreous hemorrhage occurs when extravasated blood enters here often due to three main causes: Diabetic retinopathy, vitreous detachment (with or without retinal detachment), or ocular trauma (ie foreign body or shaken baby syndrome). Visual acuity and retention of macular function depend on the extent of hemorrhage; as little as 12.5 microliters of blood can cause vision changes or painless vision loss [3].
Patients will present complaining of unilateral painless vision changes described as a hazy fog. Orbital pain and pain with extraocular movements may also be seen in cases caused by trauma. On physical exam, patients may have a decreased red reflex on ophthalmoscopic examination [4]. If left untreated, patients may experience retinal detachment, glaucoma and/or permanent vision loss.
Anticoagulation has not been shown to be a risk factor for developing vitreous hemorrhage if appropriately anticoagulated [4]. Patients on warfarin should have their INR checked before determining a need to correct coagulopathy.

Figure 3: Accumulation of blood and coagulation products (orange text, yellow arrow) can be visualized in the vitreous chamber of the eye. To better visualize this on ultrasound, maximize the gain to the highest setting.

Figure 4: Another depiction of debris and other blood products (yellow arrow) in the vitreous chamber.
Management
- Elevate the head of the bed
- Provide symptomatic treatment; nausea and vomiting may occur. Avoid prescribing nonsteroidal anti-inflammatories.
- Treat underlying cause and observe as the vitreous hemorrhage will typically clear
- Ensure follow-up with ophthalmology within 24 hours
Disposition and Case Conclusion
Following the ultrasound findings above, ophthalmology was consulted and an appointment was made several hours later that same morning for the patient to return for further evaluation.
References
- Hooker EA, Faulkner WJ, Kelly LD, Whitford RC. Prospective study of the sensitivity of the Wood’s lamp for common eye abnormalities. Emerg Med J. 2019. PMID: 30630841
- Lahham S, et al. Point-Of-Care Ultrasonography in the Diagnosis of Retinal Detachment, Vitreous Hemorrhage, and Vitreous Detachment in the Emergency Department. JAMA Netw Open. 2019 Apr;2(4):e192162. PMID: 30977855
- Thompson JT, Stoessel KM. An analysis of the effect of intravitreal blood on visual acuity. Am J Ophthalmol. 1987; PMID: 3661644
- Spraul CW, Grossniklaus HE. Vitreous Hemorrhage. Surv Ophthalmol. 1997; PMID: 9265701