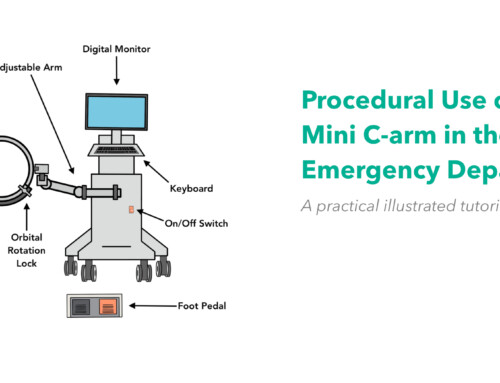
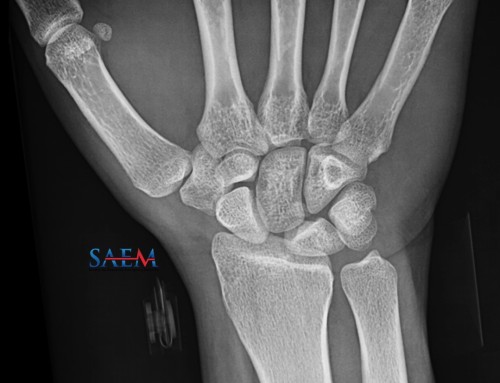
Hip fractures are an important cause of morbidity and mortality in older adults. The average age for hip fractures in the U.S. is 80 years, and a staggering 20% of women and 10% of men 1 will experience a hip fracture in their lifetime if they live to older age. This makes it a costly injury, racking up close to $15 billion per year in the U.S. alone. 2 Some hip fractures are obvious as soon as the patient rolls through the ambulance bay. Others can be subtle and require more than just a plain X-ray. This post will discuss risk factors for hip fractures, and how to diagnose and manage patients with hip fractures in the ED.
Epidemiology and Risk Factors
In young patients, hip fractures are usually associated with high speed impacts. By contrast, the primary cause of hip fractures in older adults is a simple fall from standing position. 1-year mortality following a hip fracture is high, around 16%, which is twice as high as age-matched controls who did not have a fracture. 3,4 The mortality risk is highest in the first 3 months after a fracture, in which there is a 5-8 fold higher risk of death. 1 Only half of patients who survive will return to pre-injury levels of function and be independently mobile, and 20% will need long-term care and will not be able to return home. 5
Many factors collide to put older adults at higher risk for hip fractures. Some of the risk factors are modifiable, while others are fixed:
Non Modifiable Risk Factors:6
- Female gender – 80% of all hip fractures are in women 5
- Advanced age – almost all hip fractures are in people over age 65 years, but the average age is 80 years, making it almost an exclusive injury of the very old 5
- Prior hip fracture
- Family history of hip fracture
- Low socioeconomic status
Potentially Modifiable Risk Factors:
- Osteoporosis
- Frequent falls
- Poor activity level and conditioning
- Vitamin D deficiency
- Certain medications, such as levothyroxine, which decreases bone density, and medications that reduce calcium levels, such as loop diuretics and proton pump inhibitors (PPI), and medications that increase the risk of falls due to sedation or postural hypotension.
Presentation and Diagnosis of Hip Fractures
The classic patient with a hip fracture is an older adult who has had a mechanical fall, and presents with pain in the groin area. The leg may be abducted, externally rotated, and shortened in cases of displaced fractures, or may have a normal appearance. They will have pain with any movement. You should avoid trying to range the hip if you are concerned there is a fracture, because it could worsen a displacement. During the physical exam, be sure to look for signs of other bony injuries to guide your diagnostic imaging. Feel for vertebral pain or femur pain, range their knees and check their wrists if they fell onto their hands. Also check their distal pulses. If there is a femur fracture and vascular injury, they may have diminished pulses and sensation in their feet. As with any fall, ask about headaches, loss of consciousness, and check for neck pain or external signs of head trauma. After a physical exam, the next step in diagnosis of the hip injury is plain films of the pelvis and hip.
In some cases the X-ray is negative but the patient still complains of hip or groin pain and has difficulty bearing weight. In these cases there may be an occult fracture. If they are not back to their baseline ambulatory status, then an MRI is warranted to look for occult fractures. A CT scan can also be used, but MRI is recommended if available.
Fractures are categorized as either extracapsular (inter- and sub-trochanteric), or intracapsular (those in the femoral head or neck). Intracapsular fractures tend to have more complications and do not heal as well. 6 Patients may require a hemarthroplasty for these fractures.
Management of Hip Fractures
For older patients with falls, we have several goals in the ED:
- Assess the extent of injuries: We have to ensure nothing else is missed such as a subdural, or a vertebral fracture.
- Consider the cause of the fall: It may have been mechanical, but the patient may have been less steady because of dehydration. Other times it may have been syncopal, necessitating a broader workup.
- Provide analgesia: Older adults may not be as vocal as younger patients about their need for pain medications. Typically they are not the patients you find complaining of a pain of 15 on a scale that only goes up to 10. Be sure to ask about their level of pain and treat it appropriately. Once you have obtained a neurologic exam of the extremity, you could consider a femoral nerve block (Sonosite YouTube tutorial video and a Ultrasound Podcasts tutorial) 7 or a fascia iliaca block 8, both of which can provide good analgesia. Otherwise, IV medications such as low-dose morphine with frequent reassessment and titration as needed is a good option. The nerve blocks can cut down on opiates required, which then exposes the patient to less risk of opiate-related side effects and respiratory depression.
- Consult orthopedics and admit the patient: Patients with hip fractures will typically be taken to the OR within 1-2 days. They will need hospital admission for pain control and care until their repair.
Take Home Points
- Hip fractures are common in older adults and are a huge source of loss of function and mobility and have high rates of 1-year mortality.
- Do not aggressively manipulate a patient’s hip if you suspect a fracture, as it could worsen a dislocation.
- If the hip and pelvis X-rays are negative but the patient cannot bear weight or ambulate due to hip or groin pain, consider an MRI or a CT.
- Treat the patient’s pain, and consider doing an ultrasound guided femoral nerve or fascia iliaca block.
References
- Landefeld C. Goals of care for hip fracture: promoting independence and reducing mortality. Arch Intern Med. 2011;171(20):1837-1838. [PubMed]
- Dy C, McCollister K, Lubarsky D, Lane J. An economic evaluation of a systems-based strategy to expedite surgical treatment of hip fractures. J Bone Joint Surg Am. 2011;93(14):1326-1334. [PubMed]
- Haentjens P, Magaziner J, Colón-Emeric C, et al. Meta-analysis: excess mortality after hip fracture among older women and men. Ann Intern Med. 2010;152(6):380-390. [PubMed]
- LeBlanc E, Hillier T, Pedula K, et al. Hip fracture and increased short-term but not long-term mortality in healthy older women. Arch Intern Med. 2011;171(20):1831-1837. [PubMed]
- Parker M, Johansen A. Hip fracture. BMJ. 2006;333(7557):27-30. [PubMed]
- LeBlanc K, Muncie H, LeBlanc L. Hip fracture: diagnosis, treatment, and secondary prevention. Am Fam Physician. 2014;89(12):945-951. [PubMed]
- Beaudoin F, Nagdev A, Merchant R, Becker B. Ultrasound-guided femoral nerve blocks in elderly patients with hip fractures. Am J Emerg Med. 2010;28(1):76-81. [PubMed]
- Ritcey B, Pageau P, Woo M, Perry J. Regional Nerve Blocks For Hip and Femoral Neck Fractures in the Emergency Department: A Systematic Review. CJEM. 2016;18(1):37-47. [PubMed]