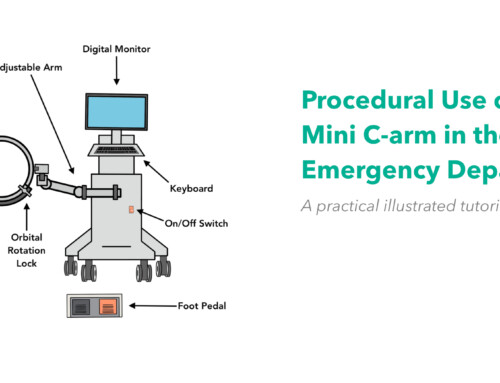
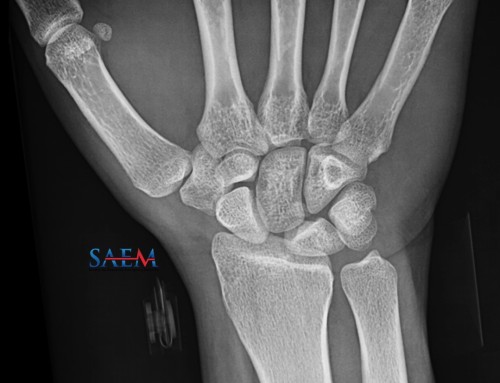
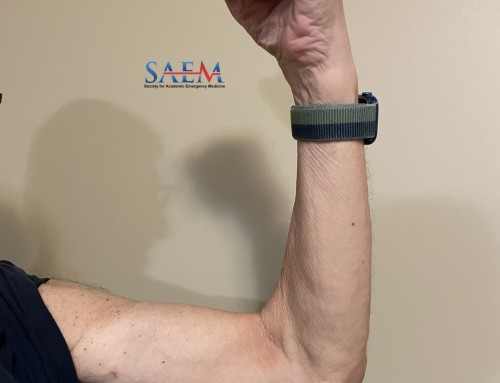
Image 1. Case courtesy of Radswiki, Radiopaedia.org
A 26 year-old male presents with new medial right knee pain after twisting his knee playing soccer 3 weeks ago. His initial pain has since resolved.
What is your diagnosis? What examination findings should you expect? What associated diagnoses should you assess for? What is your management in the emergency department?
References:
- Mendes, L., Pretterklieber, M., Cho, J., Garcia, G., Resnick, D. and Chung, C. (2006). Pellegrini–Stieda disease: a heterogeneous disorder not synonymous with ossification/calcification of the tibial collateral ligament—anatomic and imaging investigation. Skeletal Radiology, 35(12), pp.916-922. PMID: 16988801
- Weaver, M. and Sherman, A. (2020). Pellegrini Stieda Disease. [online] Ncbi.nlm.nih.gov. PMID: 30570968