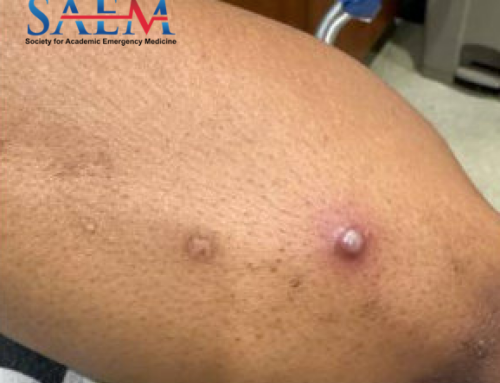
Case: A 32-year-old male with a past medical history of diabetes presents with a 1 month history of finger pain after slamming his finger in a car door. 2 weeks after the initial incident he presented to the emergency department for worsening pain and received x-rays that were negative for acute fracture. Today he presents reporting pain radiating up the hand, arm, and into the shoulder, with associated chills. His labs are significant for hyperglycemia, hyponatremia, and an elevated erythrocyte sedimentation rate and c-reactive protein. His x-ray is seen here (figure 1 image courtesy of Daniel Rogan, MD). What is the diagnosis?
Case: A 32-year-old male with a past medical history of diabetes presents with a 1 month history of finger pain after slamming his finger in a car door. 2 weeks after the initial incident he presented to the emergency department for worsening pain and received x-rays that were negative for acute fracture. Today he presents reporting pain radiating up the hand, arm, and into the shoulder, with associated chills. His labs are significant for hyperglycemia, hyponatremia, and an elevated erythrocyte sedimentation rate and c-reactive protein. His x-ray is seen here (figure 1 image courtesy of Daniel Rogan, MD). What is the diagnosis?
Acute Osteomyelitis
Explanation

Figure 2: AP x-ray of hand. Note the demineralization of the long digit’s distal phalanx. Image courtesy of Daniel Rogan, MD.
Acute osteomyelitis is an infection of the bone or bone marrow. Most often, osteomyelitis is caused by direct extension of infected adjacent soft tissues, but can also be caused by hematogenous spread. Some epidemiology:
- 1/675 hospital admissions [1]
- Higher incidence in men
- Rates increase with age
- Risk factors: diabetes, peripheral vascular disease [2]
Acute Osteomyelitis: Diagnosis
Acute osteomyelitis can be difficult to diagnose, and must be distinguished from other infectious causes of pain and swelling, such as felon, flexor tenosynovitis, simple cellulitis, and septic arthritis. Some pearls [3, 4]:
- Probing to bone on physical examination is 66% sensitive, 85% specific for acute osteomyelitis.
- X-rays are 43-75% sensitive for acute osteomyelitis.
- Abnormal inflammatory markers (WBC, ESR, CRP) are helpful but not diagnostic.
- MRI is the most sensitive and specific test for acute osteomyelitis, with sensitivities of 82-100% and specificities of 60-90%.
Acute Osteomyelitis: Management
Source control is imperative. This includes [4]:
- Surgical management and resection of infected bone
- Risk factor control
- Prolonged antibiotics
- Culture prior to antibiotics is ideal, but in the unstable patient empiric antibiotics are reasonable.
- A popular choice for empiric antibiotics is vancomycin and third generation cephalosporin.
Case Conclusion
The patient was started on vancomycin and pipercillin-tazobactam. His arm was elevated and he was given insulin and IV fluids in addition to antibiotics. He was taken to the operating room with plastic surgery the next day, where he was found to have a severe felon with subcutaneous abscess and associated distal phalanx osteomyelitis. No purulence was noted in the flexor sheath. The patient underwent an uncomplicated distal phalanx amputation and recovered without complication.
Check out the Diagnose on Sight Archives.
References
- Rubin RJ, Harrington CA, Poon A, Dietrich K, Greene JA, Moiduddin A. The economic impact of Staphylococcus aureus infection in New York City hospitals. Emerging Infect. Dis. 1999 Jan-Feb;5(1):9-17. PMID: 10081667
- Kremers HM, Nwojo ME, Ransom JE, Wood-Wentz CM, Melton LJ, Huddleston PM. Trends in the epidemiology of osteomyelitis: a population-based study, 1969 to 2009. J Bone Joint Surg Am. 2015 May 20;97(10):837-45. PMID: 25995495
- Pineda C, Espinosa R, Pena A. Radiographic imaging in OM: the role of plain radiography, computed tomography, ultrasonography, magnetic resonance imaging, and scintigraphy. Semin Plast Surg. 2009; 23(2): 80-89. PMID: 20567730
- Schmitt SK. Osteomyelitis. Infect. Dis. Clin. North Am. 2017 Jun;31(2):325-338. PMID: 28483044