On a shift last week, we had a patient present with a spontaneous pneumothorax. Not only that, but it was a tension pneumothorax. Although the patient was hemodynamically stable, he was very uncomfortable and really short of breath. To give us more time to prepare for the chest tube, it was decided to perform a needle thoracostomy.
On a shift last week, we had a patient present with a spontaneous pneumothorax. Not only that, but it was a tension pneumothorax. Although the patient was hemodynamically stable, he was very uncomfortable and really short of breath. To give us more time to prepare for the chest tube, it was decided to perform a needle thoracostomy.
Before I could even ask “does anyone have a 16 gauge angiocatheter?”, one of our residents Dr. Caitlin Bilotti was already prepping the patient’s skin. Apparently she carries such an angiocath at all times with her for this very purpose! (I did the same thing during residency! I’m the firm believer that he/she would wields the equipment gets to do the procedure. Nice job, Caitlin.)
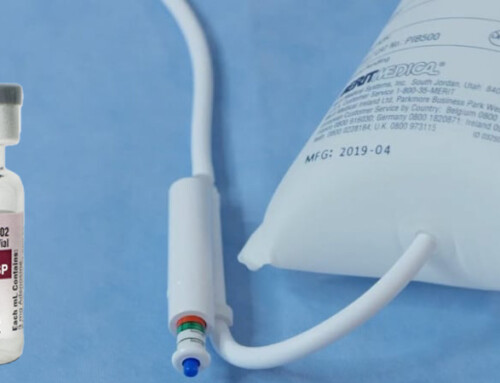
After the procedure, one of our fantastic nurses (who is also a paramedic) James Burhn showed us a trick with a three-way stopcock. Attaching a stopcock to the end of the angiocatheter serves as a means of controlling the “venting” of the pneumothorax.

He uses the stopcock to shrink the size of the pneumothorax. Start with the pneumothorax venting to the outside air. Next, have the patient take a forceful breath OUT. This maximizes the intrathoracic pressure and vents the pneumothorax air out through the stopcock. Then close the stopcock. When the patient breathes in, the outside air can no longer be sucked back into the intrathoracic cavity. After several rounds of this timed inhalation-exhalation routine with the stopcock, our patient felt significantly better.
This was a trick that James learned while serving in Iraq. Needle thoracostomies were performed as a temporizing measure, while patients were moved to safety. Also on a side note, I’ve never seen someone so excited to teach us about this neat trick. Like a kid in a candy store. Love it. Thanks, James!