Patients presenting to the ED with respiratory distress and a tracheostomy can unnerve almost any provider, and management is often fraught with preventable errors.1,2 This recognition has led to the development of treatment algorithms from groups including the U.K. National Tracheostomy Safety Project to improve the safety and quality of care for patients with tracheostomies.3 Use the ABC-Ts mnemonic to help you perform a focused tracheostomy evaluation and troubleshoot in a stepwise, systematic manner while waiting for your ENT consultant to arrive.
Patients presenting to the ED with respiratory distress and a tracheostomy can unnerve almost any provider, and management is often fraught with preventable errors.1,2 This recognition has led to the development of treatment algorithms from groups including the U.K. National Tracheostomy Safety Project to improve the safety and quality of care for patients with tracheostomies.3 Use the ABC-Ts mnemonic to help you perform a focused tracheostomy evaluation and troubleshoot in a stepwise, systematic manner while waiting for your ENT consultant to arrive.
Tracheostomy Troubleshooting Steps (ABC-Ts)
| Mnemonic | Description |
| A | A irway |
| B | B reathing (assess the mouth and stoma) |
| C | C ore Actions
|
| T | T ube
|
 A – Airway
A – Airway
- Approach the patient according to standard guidelines such as BLS/ACLS.
- Assess the patient’s tracheostomy:3,4
- Does the tube appear overtly dislodged?
- Is there is a pilot balloon, suggesting the presence of a cuff?
B – Breathing (at both the mouth and stoma)
- Look and listen to assess the patient’s breathing.
- Provide oxygen via the MOUTH.
- Most patients with a tracheostomy often have patent upper airways and can therefore be oxygenated via the oral-nasal route.
- Note: Patients with a laryngectomy will not improve with oral oxygenation attempts, because the upper airway is no longer connected to the trachea. These patients will rely on the stoma for oxygenation. If there is any doubt as to whether a patient has a laryngectomy, administer oxygen via the mouth because there is minimal harm.
- Provide oxygen via the STOMA.
- Administer high flow oxygen to the tracheostomy. If there is no tracheostomy tube in place, apply a laryngeal mask airway or pediatric face mask to oxygenate via the stoma.
- Assess ventilation with end-tidal CO2 capnography.3,5
- Caution: Do not manually bag the tracheostomy tube if there is any concern for malposition.3,5
C – Core Actions
- C annula
- Remove the inner cannula or cap/speaking valve of the tracheostomy tube as this may resolve an obstruction (e.g., from debris or secretions) and is necessary prior to inserting a suction catheter.
- Do not throw this piece away. Depending on the manufacturer you may need it to connect to the ventilator or BVM later on.5,6
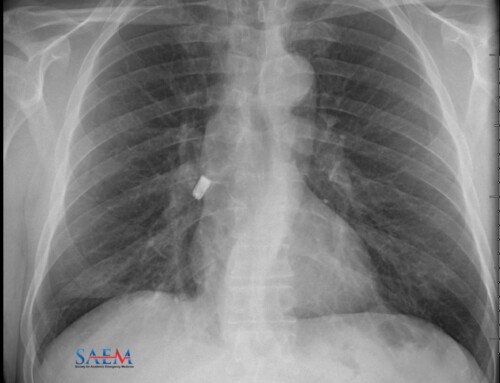
- Caution: Laryngectomy patients may not have a tracheostomy tube in place but may have other devices, such as tracheoesophageal valves (image below), which can be identified by their location along the posterior wall of the trachea. These should not be removed.3,7

- C atheter
- Pass a suction catheter through the tracheostomy tube. This will allow you to both assess patency and allow therapeutic suctioning.
- Catheter does not advance: The tube may be clogged or displaced. Continue with additional troubleshooting steps below.
- Catheter advances freely and to an appropriate depth: The tracheostomy/airway is patent.
- Caution: Do not use a bougie as a surrogate catheter because it is stiff and if the tube is displaced there is the risk for creating a false tract.3
- Pass a suction catheter through the tracheostomy tube. This will allow you to both assess patency and allow therapeutic suctioning.
- C uff
- Deflate the tracheostomy cuff because this may relieve a partial obstruction and aid in airflow.
T – Tube
- T rumped by oxygen status
- Assess if the patient is oxygenating and improving with your previous maneuvers. Oxygenation is the priority.3,4,8
- Oxygenation is adequate: You have time to assess the patient’s non-airway issues.
- Oxygenation is NOT adequate: Ensure that a cricothyrotomy setup available, and proceed with the more aggressive airway troubleshooting steps below.3,15
- Assess if the patient is oxygenating and improving with your previous maneuvers. Oxygenation is the priority.3,4,8
- T ake out the tracheostomy tube
- Removing the tracheostomy tube can be a life-saving step in decompensating patients refractory your initial stabilization maneuvers. It may be causing an obstruction.
- Upon tube removal, ensure that the patient is being oxygenated via the mouth and stoma.3
- T ube from above
- Visualize the vocal cords using video or fiberoptic laryngoscopy under ketamine to determine if oro/nasotracheal intubation is a viable option. This is analogous to the concept of an awake intubation. If you have a good view, consider adding a paralytic and passing an endotracheal tube, which should advance past the stoma.3,9–12
- T ube from below
- If the patient is not improving after maximal oxygenation attempts and can not be intubated from above, you will need to intubate the stoma ideally using a fiberoptic device. Blind attempts are less preferred, because of the risk for creating a false passage.3,13,14 If a fiberoptic device is unavailable, consider utilizing a bougie to help guide tube passage.
Frequent reassessments of airway and breathing are key
After any intervention, reassess the patient’s work of breathing and respiratory status. If the patient improves and stabilizes, you have at least temporarily addressed the patient’s airway and breathing. There is now a little time to continue with the rest of the patient’s overall assessment.
Congratulations
Congratulations to author Dr. Puja Gopal on her is winning blog post submission for the 2018 ALiEM-EEM Fellowship competition.
Image 2, Image 3