Welcome to Leg Day #4 of the SplintER Series! Ankle dislocations are an emergent condition in the Emergency Department (ED) that requires expert-level examination and management. We review the pertinent and subtle sports medicine examination and management techniques that will help you feel in control from time of presentation to disposition.
Bottom Line
- Closed ankle dislocations without any other fracture are rare.
- Posterior ankle dislocations are the most common type of ankle dislocation.
- If patients have signs of neurovascular compromise or skin tenting from a posterior dislocation, they should be reduced immediately without waiting for radiographs. With an assistant, bend the knee, plantar-flex the ankle, and apply traction with an anterior force to the heel.
- If high energy / complex fracture-dislocation, consider a post-reduction CT to ensure there are no additional injuries.
- Place patients in a short posterior leg splint ± stirrup after reduction.
- Bosworth fracture-dislocations, which will require an open reduction internal fixation, may be missed on plain film with CT imaging providing better visualization.
- Emergent orthopedics consultation should be obtained for an ankle dislocation if it is irreducible, associated with a fracture, demonstrates neurovascular compromise, or is open.
Ankle Dislocation: An Overview
Closed ankle dislocations without fractures are rare. Compared to uncomplicated fractures, the complication rate in ankle fracture-dislocations is tripled.1 Dislocations are classified based on the position of the talus relative to the tibia. Most commonly, ankle dislocations are posterior or lateral and require a high-energy mechanism.2,3 Lateral dislocations are more likely to be associated with an open fracture.
Skin tenting and neurovascular compromise are indications for immediate reduction without waiting for radiographs.4 After reducing the injury, neurovascular status should be re-confirmed, a splint should be applied, and imaging should be obtained to confirm alignment. The patient will need to be immobilized for approximately 6-9 weeks followed by physical therapy. Once rehabilitated appropriately, patients are usually able to return to their normal activities as before.5
Anatomy

The ankle is a stable joint due to the support given by the medial ligaments (deep and superficial deltoid) and lateral ligaments (anterior talofibular, calcaneofibular, posterior talofibular; Figure 1). The talus position in the mortise adds additional support. The anterior and posterior stability of the ankle is not as robust, considering that the joint capsule and surrounding musculature are supportive. In posterior ankle dislocations, for instance, when the ankle is plantar flexed it reciprocally causes the talus to be less stable in the mortise. The combination of axial, eversion, and/or inversion forces can then easily lead to the dislocation of the talus from the tibiotalar joint. 5,6
Physical Examination Findings
Document any obvious deformities, swelling, and presence of distal pulses (dorsalis pedis and posterior tibial). Compared to the lower leg, the foot will appear more posterior for posterior dislocations. Look for any breaks to the skin, which could indicate an open injury. Assess sensation at all surfaces of the foot (dorsum, plantar, lateral, medial).
Imaging

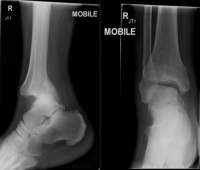
For uncomplicated ankle dislocations, there should be no additional fractures and the tibiofibular syndesmosis should not be pathologically widened. With regards to posterior dislocations, the talus is located posteriorly to the tibia and may be better visualized on lateral views (Figure 2). While plain films should be the initial imaging study, CT imaging should be considered to evaluate for concomitant injury or osteochondral fragments trapped within the joint space.5
Bosworth Fracture-Dislocation

The Bosworth fracture-dislocation is a rare entity, which is a posterior talar dislocation and displacement of the distal fibula posterior to the distal tibia, best noticed on the lateral xray. On plain film, it may initially appear as a posterior dislocation with a uni/bimalleolar fracture.7 However, it is extremely difficult to reduce as the proximal part of a fibular fracture becomes entrapped behind the lateral tibial tubercle. Reduction of the tibio-talar joint may be achieved in some circumstances; however, the fibular fragment will remain entrapped posteriorly. Given patient discomfort, positioning of lateral radiographs may not reveal the displacement. With a high degree of suspicion, CT imaging is recommended.7 Open reduction and internal fixation is necessary to achieve appropriate alignment.
Reduction Technique
Ensure the patient has received sedation and/or pain medications for comfort and to increase reduction success. Usually an assistant is needed to help with patient positioning and providing traction during the reduction procedure. When reducing any joint, the initial step is to recreate the mechanism. Knee flexion can help to remove tension on the Achilles tendon at the heel.5
- Lateral fracture-dislocations2
- Bend the knee 90°
- Plantar-flex the ankle
- Apply axial traction on the foot
- Apply lateral traction proximal to and medial pressure distal to the injury
- Posterior ankle dislocation2
- Bend the knee 90°
- Plantar-flex the ankle
- Apply axial traction on the foot
- Apply posterior traction proximal to and anterior pressure distal to the injury
Similar approaches are taken for medial and anterior ankle dislocations.
Splint
Patients should have a short leg posterior splint placed after reduction. A stirrup can provide additional stability.
Return Precautions & Post-Discharge Care
Similar to other lower extremity injuries, patients should be advised to keep their extremity elevated to reduce swelling. They should be given crutches and advised to be non-weight-bearing until re-evaluated by an orthopedist. They should be instructed regarding proper splint care and to monitor for new numbness, tingling, weakness, discoloration, or worsening pain for potential compartment syndrome. Decisions regarding DVT prophylaxis and anticoagulation should be made in conjunction with the orthopedist involved with the patient’s care.
When to Consult an Orthopedist in the Emergency Department
Depending on the extent of injuries and institutional culture, initial orthopedic consultation and follow up scheduling can vary. Patients with signs of neurovascular compromise or skin tenting from an ankle dislocation should be reduced immediately without waiting for radiographs or an orthopedics consultation. Below is a general list of when to involve orthopedics:
- Persisting neurovascular compromise despite reduction
- Open fracture-dislocation
- Concurrent fractures
- Failed reduction attempts
Expert Evaluation and Pearls: Dr. Anna Waterbrook

Associate Professor of EM, University of Arizona Associate Program Director, Sports Medicine Fellowship Team Physician for the University of Arizona
- Neurovascular exam: Ankle dislocations typically occur due to a high mechanism force. They frequently have associated fractures and neurovascular (NV) injuries – it is imperative to perform a quick but thorough NV exam upon initial presentation and monitor that status throughout the ED course. Do not delay reduction for radiographs if there is compromise.
- Soft tissue injury: Isolated dislocations can lead to significant instability due to ligamentous or cartilage injuries – there is a risk for chronic ankle instability.
- Unable to reduce: If unable to reduce the dislocation in the ED, consider a Bosworth fracture, underlying cartilage disruption, or osteochondral injury. CT imaging is recommended.
- Mimicker: Differentiate a true ankle (talar) dislocation from a subtalar dislocation, as the methods for reduction are different. Subtalar dislocations can be more difficult to reduce in the ED.
- Post-reduction care: All patients with ankle dislocations being discharged require complete instructions including splint care, monitoring for complications, and close outpatient orthopedic follow-up. Ligaments are torn in dislocations and can sometimes result in chronic ankle stability.
References
- Carragee EJ, Csongradi JJ, Bleck EE. Early complications in the operative treatment of ankle fractures. Influence of delay before operation. J Bone Joint Surg Br 1991;73(1):79–82. PMID 1991782
- Handel DA, Gaines SA. Ankle Injuries. In: Tintinalli JE, Stapczynski JS, Ma OJ, Yealy DM, Meckler GD, Cline DM, editors. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e. New York, NY: McGraw-Hill Education; 2016.
- Davenport M. Ankle [Internet]. In: Sherman SC, editor. Simon’s Emergency Orthopedics. New York, NY: McGraw-Hill Education; 2014.
- Schwartz DT. Chapter IV-1. Ankle Fractures. In: Emergency Radiology: Case Studies. New York, NY: The McGraw-Hill Companies; 2008.
- Mubark I, Anwar S, Hayward K. Closed posterior ankle dislocation without associated fractures: a case report. J Surg Case Rep 2017 [cited 2019 Apr 13];2017(8). PMID 28928920
- Agrawal AC, Raza H, Haq R. Closed posterior dislocation of the ankle without fracture. Indian J Orthop 2008;42(3):360–2. PMID 19753168
- Silverio A, Rebich E, Basso-Williams M, Vardiabasis N, Robinson M. Bosworth Ankle Fracture-Dislocation [Internet]. The Orthopod. [cited 2019 Apr 10]; Webpage available from: https://www2.aoao.org/members/news/2014winter/casereport2.html





