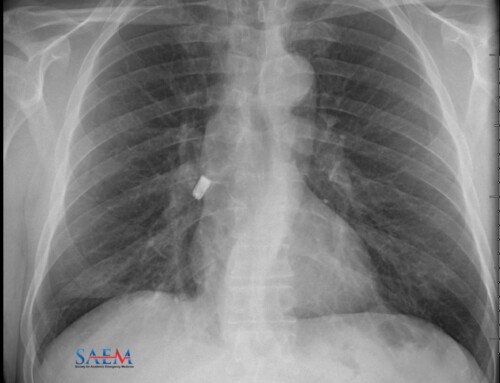
A 51-year-old female with a history of metastatic ovarian cancer on chemotherapy, malignant pleural effusions requiring repeat thoracentesis, and pulmonary embolism presented to the Emergency Department with worsening shortness of breath and dry cough. Upon arrival, she was hypoxic with an oxygen saturation level of 75% on room air. She was tachycardic, tachypneic, and her blood pressure was 125/56 mmHg. Labs revealed only a mild anemia (Hgb: 10.2). It was determined that her symptoms were secondary to recurrent right-sided malignant pleural effusions. Her presenting chest X-ray is pictured above (Image 1: Author’s own image).
Because of the patient’s debilitating symptomatology, a right-sided bedside thoracentesis was performed. 1.5 L of thin, dark brown fluid was removed and after the procedure, the patient stated she felt much better. Repeat vital signs after thoracentesis revealed: HR 105 bpm, RR 18 rpm, O2 saturation of 98% on room air. Blood pressure remained stable. A repeat chest x-ray was performed:

Image 2: Patient’s x-ray after thoracentesis (author’s own image).
References
Want more visual diagnosis? We see you! Check out ALiEM’s archives for Diagnose on Sight, SAEM’s Clinical Images, and ACMT’s Visual Pearls.
- Doelken P, Sahn SA. Trapped lung. Semin Respir Crit Care Med. 2001;22(6):631-636. PMID: 16088707
- Huggins JT, Doelken P, Sahn SA. The unexpandable lung. F1000 Med Rep. 2010;2:77. PMID: 21173837
- Divietro M, Huggins J, Doelken P, Gurung P, Kaiser L, Sahn S. Prevalence and causes of unexpandable lung over a ten-year period. Chest. 2011;140:700A.
- Huggins JT, Sahn SA, Heidecker J, Ravenel JG, Doelken P. Characteristics of trapped lung: pleural fluid analysis, manometry, and air-contrast chest CT. Chest. 2007;131(1):206-213. PMID: 17218577
- Doelken P. Clinical implications of unexpandable lung due to pleural disease. Am J Med Sci 2008; 335:21 PMID: 18195579
- Khan H, Fernandez-Perez E R, Caples S M. Post-thoracentesis trapped lung. J Postgrad Med 2007;53:119-20. PMID: 17495380
- Cantey EP, Walter JM, Corbridge T, Barsuk JH. Complications of thoracentesis: incidence, risk factors, and strategies for prevention. Curr Opin Pulm Med. 2016;22(4):378-385. PMID: 27093476