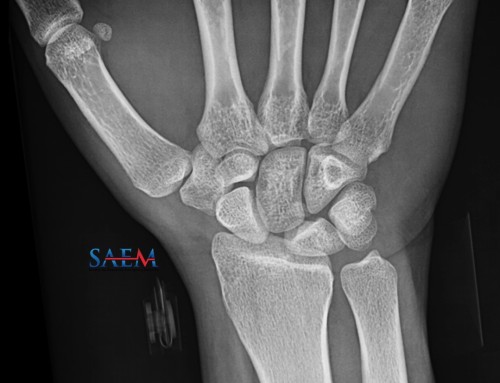
A patient comes into your department with an obvious shoulder dislocation. You know you can easily reduce the shoulder and have the patient discharged before the orthopedic consultant calls back. But what if there is a fracture? Do you need to get that plain film before popping it back into place?
A patient comes into your department with an obvious shoulder dislocation. You know you can easily reduce the shoulder and have the patient discharged before the orthopedic consultant calls back. But what if there is a fracture? Do you need to get that plain film before popping it back into place?
The reduction of a shoulder dislocation is one of those procedures that we as emergency physicians relish. The patient has a problem, we can fix it, and the patient goes home. But this can be a time consuming process when you take into account assessing the patient, getting pre-reduction films, providing conscious sedation, getting post-reduction films, and discharging the patient. I won’t go into methods of reducing the shoulder or whether or not sedation is needed. But is it possible to shave time off of these visits and improve throughput?
Pre-reduction radiographs in clinically evident anterior shoulder dislocation1
A prospective study from Canada assessed if emergency physicians can accurately identify anterior shoulder dislocations not needing a pre-reduction film. A total of 40 cases were included, all of which (100%) had a pre-reduction film that did NOT affect the management. It was interesting to note that pre-reduction films added 29.6 +/- 12.68 minutes to length of stay.
Pre-reduction films in blunt trauma2
This was a prospective, observational study that had 104 patients with shoulder dislocations, 28 were recurrent with atraumatic mechanism and 76 had no prior dislocations or had a blunt mechanism of injury. In this study, physicians were able to accurately assess all recurrent dislocations and 98% of the other group. Incorrect assessments were found in patients that had fractures. The authors concluded that pre-reduction films should be obtained in patients with blunt trauma and post-reduction films should be performed for those with a fracture-dislocation. Neither pre-reduction nor post-reduction films were likely to affect management of recurrent dislocations with atraumatic mechanism of injury.
So, what about these fractures? How often do they occur?
How common are fractures associated with dislocations?3
A retrospective study was conducted to examine the percent of dislocations that had an associated fracture as a function of age. A total of 7,209 patients had dislocations with 6.5% having an associated fracture. The authors found that the older the patient was, the more likely that there was an associated fracture. Through the third decade of life, patients have < 1% chance of having a fracture-dislocation. The percentage jumps to 2.6% in the fourth decade and 4.6% in the fifth decade, and then the percentages continue to rise. The study’s conclusion was that pre-reduction x-rays might not be necessary in the third decade of life or younger.
Wouldn’t it be nice if there were some sort of decision rule for these patients?
Quebec decision rule for radiography in shoulder dislocation4
In this prospectively derived clinical decision rule, the authors were looking to reduce the number of pre-reduction and post-reduction films in anterior shoulder dislocation. An algorithm was developed with a sensitivity of 100%, specificity of 34.2% and a negative predictive value of 99.2%, based on four at-risk factors:
- Age ≥40 years
- Mechanism (MVC, assault, sporting injury, fall from greater than patient’s height)
- Presence of humeral ecchymosis
- First episode of dislocation
This algorithm reduced the number of pre-reduction films by 28% and post-reduction films by 82%. It should be noted, however, all patients in the study had a GCS of 15 and that this clinical decision rule has yet to be validated. In fact, this rule failed validation in an Australian study.5
Bottom line
If your patient presents with a dislocated shoulder for the tenth time with no injury, you probably don’t need any films at all. If there is any trauma, or any doubt on your part, go ahead and get the pre-reduction film.