SAEM Clinical Images Series: Male Weightlifter with Chest Pain

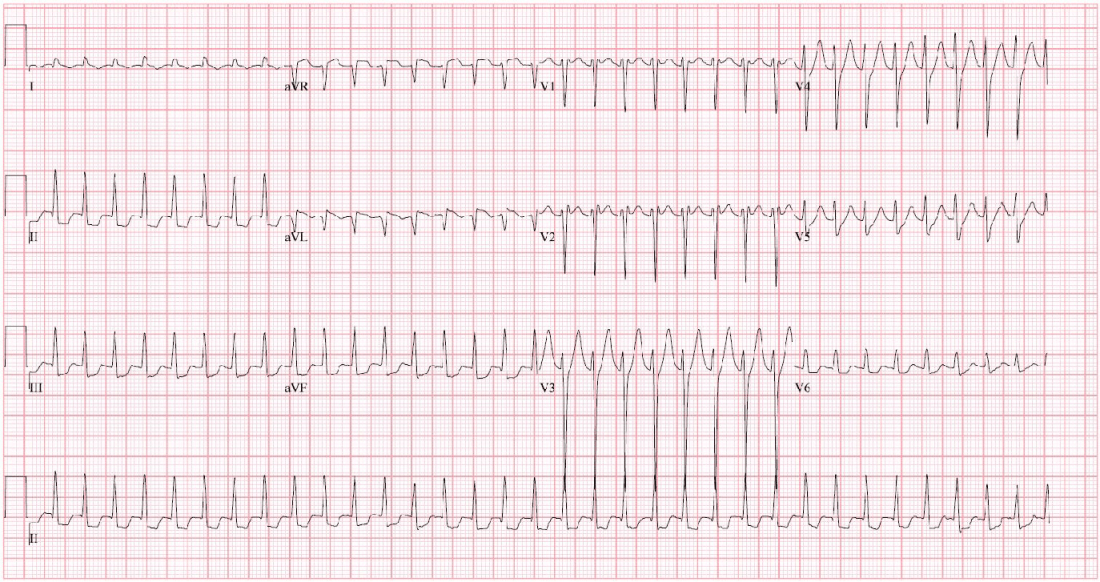
An otherwise healthy 45-year-old male presented to the emergency department (ED) with substernal chest pain radiating down his left arm over the previous two days. On the first day of symptoms, his pain began several hours after using a new pre-workout supplement and weightlifting. The symptoms lasted for a few hours and self-resolved. The pain returned the following day under the same conditions, although this time persistent, which brought him in for evaluation. Associated symptoms included shortness of breath, nausea, and one episode of emesis. He denied pleuritic pain, lower extremity edema, hemoptysis, syncope, cough, or chest wall trauma. On further history, he reported prior use of anabolic steroids, with the last being six weeks prior to presentation. It was unclear what were the contents of the pre-workout supplement, but he denied any tobacco or illicit drug use. Notably, he had a significant family history of heart disease with his father having undergone coronary bypass at age 47. His initial ECG (Image 1) and interval ECG (Image 2) are shown.