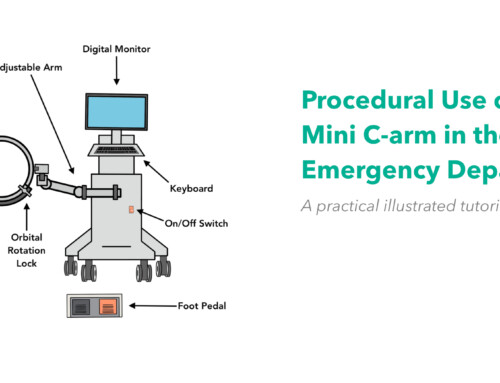
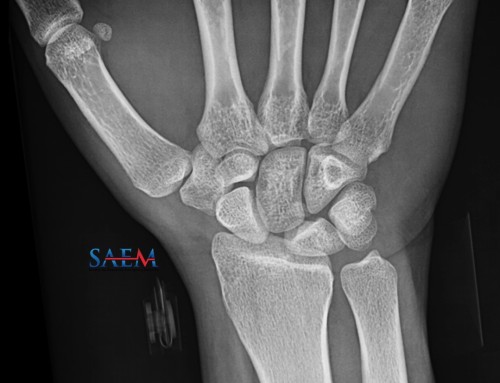
Case: An 18 year old male presents after a single gunshot wound to his left calf. He complains of pressure-like pain near the wound and sensory numbness below his left knee. On examination, the left leg is tense. He has no dorsalis pedis pulse. Based on the history, exam, and findings in the image, which of the following is true regarding this diagnosis?
Case: An 18 year old male presents after a single gunshot wound to his left calf. He complains of pressure-like pain near the wound and sensory numbness below his left knee. On examination, the left leg is tense. He has no dorsalis pedis pulse. Based on the history, exam, and findings in the image, which of the following is true regarding this diagnosis?
Poll Results
[plot id=”1″] [su_spoiler title=”Answer” style=”fancy” icon=”caret”]Diagnosis can be made by clinical exam alone
Explanation
This patient’s lower extremity numbness and pain were caused by compartment syndrome, which occurs when elevated pressure within fascial compartments causes ischemic necrosis of muscle. This challenging diagnosis can be made in two ways:
Clinical Exam1
- Pain out of proportion – the most common and possibly most sensitive sign
- Motor weakness – classic, but limited by pain and injuries
- Palpation – not sensitive
- Pain on passive stretch – not scientifically validated
- Sensory deficits – limited specificity
Measurement of Compartment Pressure
Traditionally, absolute compartment pressure >30 mmHg or perfusion pressure (diastolic blood pressure – compartment pressure) <30 mmHg have been thresholds for diagnosing compartment syndrome. But recent evidence shows that this may not be a valid diagnostic criteria alone.
Absolute pressure >30 mmHg has a high false positive rate.* Perfusion pressure <30 mmHg has been shown in multiple studies to have a high false-positive rate and poor specificity of ~65%.1 Two studies showed that no patient with measurements qualifying for fasciotomy actually needed the procedure.2,3 Clinicians should consider this important diagnosis while remembering that bedside pressure measurements are imperfect.
Master Clinician Bedside Pearls
Eric Silman, MD
Assistant Clinical Professor
Department of Emergency Medicine
University of California San Francisco
@Silmonster[/su_spoiler]