We are very excited this month to bring you our second Global Journal Club, co-hosted by the team here at ALiEM and the editorial board at the Annals of Emergency Medicine. This month, we are changing things up! We will be providing you, our readers, with a clinical vignette and related journal club questions today at the beginning of the week.The discussion will be held asynchronously starting today through Thursday (for 4 days). Respond by blog comment below or tweet (#ALiEMJC).
We are very excited this month to bring you our second Global Journal Club, co-hosted by the team here at ALiEM and the editorial board at the Annals of Emergency Medicine. This month, we are changing things up! We will be providing you, our readers, with a clinical vignette and related journal club questions today at the beginning of the week.The discussion will be held asynchronously starting today through Thursday (for 4 days). Respond by blog comment below or tweet (#ALiEMJC).
On Wednesday, January 22, 2014 at 11 am PST (2 pm EST), we will be hosting a 30-minute live Google Hangout with Drs. Jeff Perry and Ian Stiell. The video will be embedded on this page. During this period, you will be able to tweet by using the #ALiEMJC hashtag and post comment in the blog comment section below.
Clinical Vignette
It is 8 pm on a Wednesday night. Your shift ends in two hours, and you are just beginning the latter half of your shift in the quick-care area.
Your next patient is a 24-year-old female with a headache.
She discloses that she has had the worst headache of her life occur about 3 hours ago. Her husband explains that she is not a ‘complainer’ and that he is quite worried because the headache occurred quite quickly, peaking within a hour of its onset. She doesn’t usually get headaches. In the ED, she has vomited once. She is afebrile, non-toxic in appearance, and although she complains of mild neck pain, you do not note any frank nuchal rigidity. She has mild photophobia and phonophobia, but there are no focal neurologic deficits when you examine her.
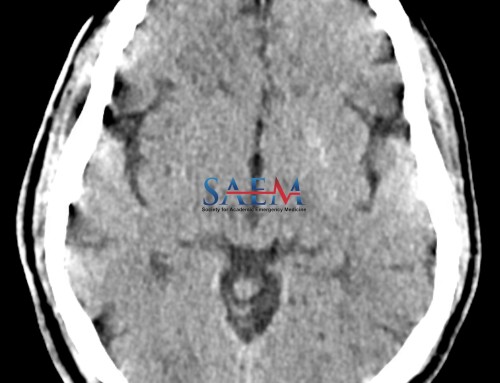
She is very relieved to see that you are empathetic to her concerns, and you quickly arrange a CT scan to rule out a subarachnoid hemorrhage (SAH). In the meantime, you also provide her with analgesics and an antiemetic.
The 64-slice CT scan is read by the second-year radiology resident on call as negative for SAH. Just as you are about to consent the patient for a lumbar puncture (LP), a senior resident in the department asks you: “Wasn’t there a study by Perry et al. that suggested you don’t need to do an LP anymore? Can’t you just rule out SAH with the clinical decision rule that they proposed?”
Featured Journal Club paper
Perry JJ, Stiell IG, Sivilotti ML, Bullard MJ, Hohl CM, Sutherland J, Émond M, Worster A, Lee JS, Mackey D, Pauls M, Lesiuk H, Symington C, Wells GA. Clinical decision rules to rule out subarachnoid hemorrhage for acute headache. JAMA. 2013 Sep 25;310(12):1248-55. PubMed PMID: 24065011
Live Google Hangout with Authors Dr. Perry and Stiell
Edited Podcast Version of Google Hangout
Abstract
IMPORTANCE: Three clinical decision rules were previously derived to identify patients with headache requiring investigations to rule out subarachnoid hemorrhage.
OBJECTIVE: To assess the accuracy, reliability, acceptability, and potential refinement (ie, to improve sensitivity or specificity) of these rules in a new cohort of patients with headache.
DESIGN, SETTING, AND PATIENTS:Multicenter cohort study conducted at 10 university-affiliated Canadian tertiary care emergency departments from April 2006 to July 2010. Enrolled patients were 2131 adults with a headache peaking within 1 hour and no neurologic deficits. Physicians completed data forms after assessing eligible patients prior to investigations.
MAIN OUTCOMES AND MEASURES:
Subarachnoid hemorrhage, defined as (1) subarachnoid blood on computed tomography scan; (2) xanthochromia in cerebrospinal fluid; or (3) red blood cells in the final tube of cerebrospinal fluid, with positive angiography findings.
RESULTS: Of the 2131 enrolled patients, 132 (6.2%) had subarachnoid hemorrhage. The decision rule including any of age 40 years or older, neck pain or stiffness, witnessed loss of consciousness, or onset during exertion had 98.5% (95% CI, 94.6%-99.6%) sensitivity and 27.5% (95% CI, 25.6%-29.5%) specificity for subarachnoid hemorrhage. Adding “thunderclap headache” (ie, instantly peaking pain) and “limited neck flexion on examination” resulted in the Ottawa SAH Rule, with 100% (95% CI, 97.2%-100.0%) sensitivity and 15.3% (95% CI, 13.8%-16.9%) specificity.
CONCLUSIONS AND RELEVANCE: Among patients presenting to the emergency department with acute nontraumatic headache that reached maximal intensity within 1 hour and who had normal neurologic examination findings, the Ottawa SAH Rule was highly sensitive for identifying subarachnoid hemorrhage. These findings apply only to patients with these specific clinical characteristics and require additional evaluation in implementation studies before the rule is applied in routine clinical care.
Notable tables from the paper (Box 1 and 2)
| Rule 1 | Investigate if ≥ 1 high-risk findings present: 1. Age ≥ 40 years 2. Neck pain or stiffness 3. Witnessed loss of consciousness 4. Onset during exertion |
| Rule 2 | Investigate if ≥1 high-risk findings present: 1. Age ≥ 45 years 2. Arrival by ambulance 3. Vomiting (≥1 episode) 4. Diastolic blood pressure ≥ 100 mmHg |
| Rule 3 | Investigated if ≥1 high-risk findings present: 1. Age 45-55 years 2. Neck pain or stiffness 3. Arrival by ambulance 4. Systolic blood pressure ≥ 160 mmHg |
| Ottawa SAH Rule | For alert patients >15 years with new, severe nontraumatic headache reaching maximum intensity within 1 hour: Investigate if ≥1 high-risk variables present: Not for patient with new neurologic deficits, previous aneurysms, SAH, brain tumors, or history of recurrent headaches (≥3 episodes over the course of ≥6 months) |
Featured Questions for our Audience
Two questions were selected from those published in this month’s Journal Club questions published in Annals of EM [free PDF] and two questions posed by the ALiEM team to address more issues of how HOW and WHETHER these results change practice (i.e. knowledge translation). Of course if you have additional questions, feel free to pose them!
Annals of EM questions
In this article, 26% of patients arrived by ambulance, and “arrival by ambulance” was one of the 4 variables in rule 2. The inclusion of this variable suggests that patients arriving by ambulance are at greater risk for subarachnoid hemorrhage.
In some settings, patients arriving by ambulance are automatically triaged to higher-acuity beds.
- Q1: How might the patient’ s location in the ED when treated by the clinician affect the evaluation that he receives?
- Q2: Why might this be especially important for EDs that employ midlevel providers or resident moonlighters to staff the low-acuity areas?
ALiEM Questions
- Q3: In your clinical practice, what information do you provide when counseling patients about the role of lumbar punctures for ruling out SAH?
- Q4: In a teaching centre, how do you integrate learning with patient care? Is the read of a second year radiology resident sufficient for ruling out SAH in this patient? Does this paper answer this question?
Please participate the journal club by answering either on the ALiEM blog comments below or by tweeting us using the hashtag #ALiEMJC. When responding, please denote the question to which you are responding by writing Q1, Q2, Q3, or Q4. For example:
Q4: Our reads are usually double-checked by attending radiologists in the morning.
We reserve the right to use any and all tweets to #ALiEMJC and comments below in a commentary piece for an Annals of Emergency Medicine publication as a curated conclusion piece for this global journal club. Your comments will be attributed, and we thank-you in advance for your contributions.
UPDATE 7/17/14
The curated responses from discussions on the various platforms have been published in Annals of EM: PMID 24951414