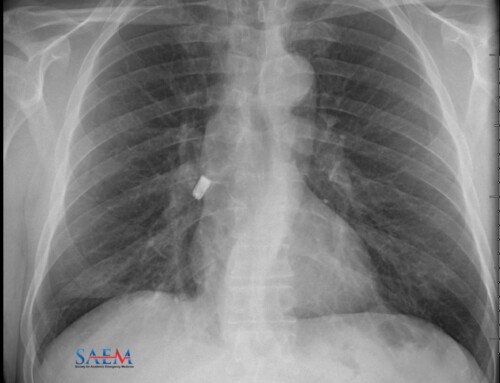
Figure 1: Photo by Tim Bish on Unsplash
Paramedics bring in a 5-month-old boy in respiratory distress. He’s crying furiously and has normal tone and color. Thick, copious secretions are coming from his nose. He is tachypneic with diffuse wheezes, crackles, retractions, and nasal flaring. His respiratory rate is 70 and his oxygen saturation is 88% on room air. Would you order a chest radiograph (CXR) for this child?
CXRs are routinely obtained in adults with respiratory symptoms. Children, however, are more sensitive to radiation and can have multiple respiratory infections every year. CXRs can increase cost, length of stay, and may not always be necessary.
This post presents some guidelines on when (and when not) to get a CXR in pediatric patients.
Bronchiolitis
The American Academy of Pediatrics (AAP) has clear guidelines for bronchiolitis:
“When clinicians diagnose bronchiolitis on the basis of history and physical examination findings, radiographic or laboratory studies should not be obtained routinely.”
Evidence quality: B; recommendation strength: strong.
Most children with bronchiolitis will have abnormal findings on CXR, but there is no evidence that the abnormalities correlate with disease severity. In addition, children who get a CXR are more likely to receive antibiotics without a change in outcome [1].
The AAP recommends reserving CXRs for bronchiolitis cases in which:
- The patient requires ICU admission
- Signs of airway complications, such as pneumothorax, are present [2]
Asthma
The National Asthma Education and Prevention Program advises against CXRs for routine assessment of acute asthma exacerbations. However, they do recommend them to evaluate for alternative diagnoses, such as pneumothorax, pneumomediastinum, or congestive heart failure [3].
Pneumonia
According to the World Health Organization, diagnosing pneumonia in children 2 months to under 5 years old does not require a CXR [4]:

CXRs have a 99% negative predictive value for ruling-out bacterial pneumonia [5]. But does a positive CXR mean the child has a bacterial pneumonia that requires antibiotics? Most often, the answer is no.
In a large study of children hospitalized with radiographic evidence of pneumonia, bacteria were only found in 15% [6]. Because CXRs do not reliably differentiate bacterial from viral pneumonia, they have limited value [7].
In 2011, the Infectious Diseases Society of America and the Pediatric Infectious Diseases Society published a guideline for CXRs in suspected pneumonia:
“Routine chest radiographs are not necessary for the confirmation of suspected community acquired pneumonia (CAP) in patients well enough to be treated in the outpatient setting (after evaluation in the office, clinic, or emergency department setting).”
Strong recommendation; high-quality evidence.
However, these organizations do recommend getting CXRs in patients with suspected hypoxemia, significant respiratory distress (in the absence of straightforward bronchiolitis), and failed initial antibiotic therapy to identify complications of pneumonia such as parapneumonic effusions, necrotizing pneumonia, or pneumothorax [7].
Lung ultrasound could be considered as an alternative to CXRs for diagnosing pneumonia.
Indications for a CXR
Though there are no national guidelines summarizing indications for CXRs, some experts recommend the following:
- First-time wheeze – to evaluate for alternative diagnoses in a child without a known history of asthma, though this is controversial [8]
- Unilateral findings – to evaluate for foreign body
- Unexplained respiratory distress – to evaluate for pneumothorax, pleural effusion, foreign body, etc.
- Recent diagnosis of pneumonia with persistent symptoms – to evaluate for complications of pneumonia such as empyema or abscess
- Afebrile upper respiratory infection for several days followed by fever – to evaluate for pneumonia and its complications
Communicating radiation risk to parents
Children are more susceptible to the harmful effects of radiation because their tissues are developing and they have a longer life expectancy. If a chest radiograph is indicated, it is worth emphasizing to parents that the benefits outweigh the risks. It may also be helpful to provide certain benchmarks – for example, a CXR is equivalent to about 3 days of exposure to natural radiation [9].
Summary
| Bronchiolitis | Asthma | Pneumonia | Foreign body | Unknown | |
|---|---|---|---|---|---|
| No CXR | Simple bronchiolitis | Uncomplicated asthma exacerbation | Suspected CAP and plan to discharge | ||
| CXR | ICU admission Signs of airway compromise (e.g. pneumothorax) | Concern for other etiology (e.g. pneumothorax, pneumomediastinum, congestive heart failure) | Hypoxemia Significant respiratory distress Failed initial antibiotic treatment | Indicated (though only 68% sensitive and 67% specific for tracheobronchial foreign body [10]) | Indicated (to identify pneumothorax, pleural effusion, foreign body, etc.) |
Table 1: Indications for CXRs based on suspected etiology
There are some situations where CXRs are helpful, but they are often not indicated.
Irradiation does not cure respiratory distress, and unnecessary radiation can lead to increased antibiotic use and harm to patients.
Returning to the 5-month-old boy with copious nasal secretions:
- His parents report he is on day four of illness, was born full-term, and has no medical problems. Based on history and physical exam, he is presumed to have bronchiolitis.
- In accordance with the AAP guidelines, a CXR is not obtained.
- His nose is suctioned using saline and an olive tip aspirator and he is given acetaminophen. His respiratory rate and oxygen saturation improve to 40 and 97%. He continues to have scattered wheezes and crackles, but now breastfeeds comfortably and has only intermittent intercostal retractions.
- After an hour of observation, his exam remains unchanged and he is discharged home with nasal suctioning and return precautions.
References
- Silver AH, Nazif JM. Bronchiolitis. Pediatrics Review. 2019;40(11):568-576. PMID: 31676530
- Ralston SL, Lieberthal AS, Meissner HC, et al. Clinical practice guideline: the diagnosis, management, and prevention of bronchiolitis. Pediatrics. 2014;134(5):e1474-502. PMID: 25349312
- National Asthma Education and Prevention Program, Third Expert Panel on the Diagnosis and Management of Asthma. Expert Panel Report 3: Guidelines for the Diagnosis and Management of Asthma. Bethesda (MD): National Heart, Lung, and Blood Institute (US); 2007: Section 5, Managing Exacerbations of Asthma. Available at: https://www.ncbi.nlm.nih.gov/books/NBK7232/. Accessed April 27, 2020.
- World Health Organization. Revised WHO classification and treatment of childhood pneumonia at health facilities. Geneva: World Health Organization; 2014. Available at: https://www.who.int/maternal_child_adolescent/documents/child-pneumonia-treatment/en/. Accessed April 27, 2020.
- Lipsett SC, Monuteaux MC, Bachur RG, et al. Negative Chest Radiography and Risk of Pneumonia. Pediatrics. 2018;142(3). PMID: 30154120
- Jain S, Williams DJ, Arnold SR, et al. Community-Acquired Pneumonia Requiring Hospitalization among U.S. Children. NEJM.2015;372(9):835-845. PMID: 25714161
- Bradley JS, Byington CL, Shah SS, et al. The Management of Community-Acquired Pneumonia in Infants and Children Older Than 3 Months of Age: Clinical Practice Guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America. Clinical Infectious Diseases. 2011;53(7):e25-76. PMID: 21880587
- Patel NH, Hassoun A, Chao JH. The Practice of Obtaining a Chest X-Ray in Pediatric Patients Presenting With Their First Episode of Wheezing in the Emergency Department: A Survey of Attending Physicians. Pediatric Emergency Care. 2020;36(1):16–20. PMID: 31851079
- World Health Organization. Communicating radiation risks in paediatric imaging. Geneva: World Health Organization; 2016. Available at: https://www.who.int/ionizing_radiation/pub_meet/radiation-risks-paediatric-imaging/en/. Accessed April 27, 2020.
- Svedström E, Puhakka H, Kero P. How accurate is chest radiography in the diagnosis of tracheobronchial foreign bodies in children? Pediatric Radiology. 1989;19(8):520-522. PMID: 2797935