SAEM Clinical Image Series: Pediatric Rash
A previously healthy 8-year-old female presents to the pediatric emergency department due to a rash. Her symptoms started three days prior to presentation with a painful rash on her lower extremities. The rash subsequently spread to the buttocks and upper extremities, and she developed intermittent diffuse abdominal pain, a nonproductive cough, and pharyngitis. The patient denies subjective fever. Known sick contacts include the patient’s mother, who tested positive for COVID-19 two and a half weeks prior. Vitals: T 98.5°F; HR 93; BP 115/68; RR 16; O2 sat 100% on room air Constitutional: Well-developed and in no acute distress HEENT: Normocephalic, atraumatic; moist mucus membranes; no conjunctival injection; posterior pharyngeal erythema without exudates; tonsils are three bilaterally; lips are not cracked; no “strawberry tongue”; Neck: Normal range of motion; no lymphadenopathy Cardiovascular: Regular rate and rhythm; normal heart sounds and pulses Pulmonary: Effort is normal; normal breath sounds; no wheezing Abdominal: Abdomen is flat; minimal tenderness to palpation without guarding; no organomegaly Skin: Diffuse petechial rash and painful, palpable, nonblanching purpura in the dependent regions (most notable on the buttocks and lower extremities) COVID-19: Detected Complete blood count (CBC): WBC 10K, hemoglobin 13, platelets 469 Comprehensive metabolic panel (CMP): Na 138, K 4.1, Cl 103, CO2 26, BUN 7, Cr 0.38, Glucose 94, ALT 23, AST 26, Albumin 4.5 Lipase: 10 Urinalysis (UA): Normal C-reactive protein (CRP): 3.4 Erythrocyte sedimentation rate (ESR): 24 Procalcitonin: 0.03 Fibrinogen: 363 BNP: <10 Troponin: 0.00 Ferritin: 83 Triglycerides: 37 Immunoglobulin A (IgA) Vasculitis. This patient presented with palpable purpura and petechiae without the presence of thrombocytopenia, as well as diffuse abdominal pain. The majority of cases of IgA Vasculitis are preceded by a respiratory pathogen, with the most common being streptococcus, staphylococcus, and parainfluenza virus. Although not well-documented due to its recent conception, COVID-19 is likely to be the cause of this patient’s vasculitis. Usual management of IgA Vasculitis is supportive care, with admission and specialty referral for complications including intussusception and glomerular involvement. Given the severity of the differential diagnoses, this patient was admitted to the hospital for observation and discharged the following day with close follow-up Images and cases from the Society of Academic Emergency Medicine (SAEM) Clinical Images Exhibit at the 2021 SAEM Annual Meeting | Copyrighted by SAEM 2021 – all rights reserved. View other cases from this Clinical Image Series on ALiEM.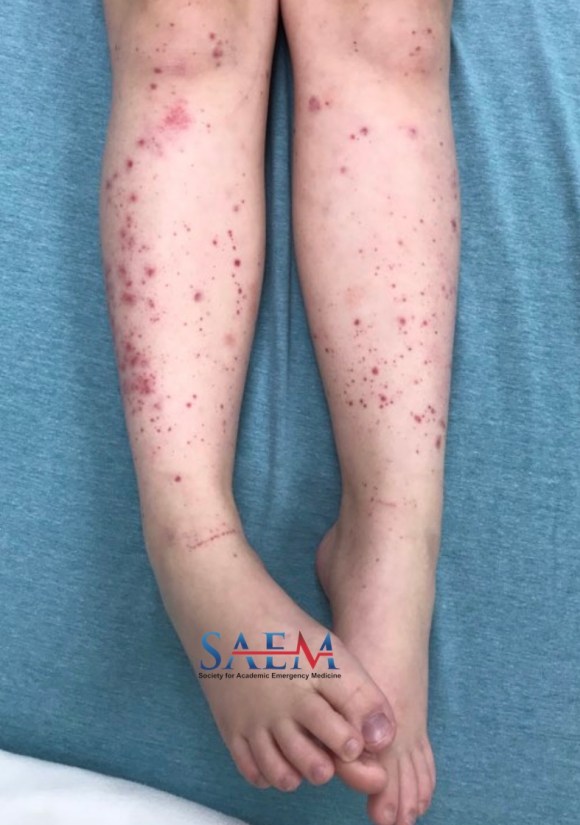
Take-Home Points
Copyright





 The novel coronavirus pandemic (COVID-19) resulted in the cancellation of educational experiences for emergency medicine (EM) residents at many institutions, including emergency medical services (EMS) ambulance ride alongs. The Accreditation for the Council of Graduate Medical Education (ACGME) requires that residents have educational experiences related to EMS, emergency preparedness, and disaster medicine. EMS experiences must include ground unit runs, direct medical oversight, and participation in multi-casualty incident drills [1]. There are few dedicated EMS curricula published in the literature, and those in existence incorporate physical ride-alongs [2].
The novel coronavirus pandemic (COVID-19) resulted in the cancellation of educational experiences for emergency medicine (EM) residents at many institutions, including emergency medical services (EMS) ambulance ride alongs. The Accreditation for the Council of Graduate Medical Education (ACGME) requires that residents have educational experiences related to EMS, emergency preparedness, and disaster medicine. EMS experiences must include ground unit runs, direct medical oversight, and participation in multi-casualty incident drills [1]. There are few dedicated EMS curricula published in the literature, and those in existence incorporate physical ride-alongs [2]. As the COVID-19 pandemic continues to unravel, the role of hydroxychloroquine (HCQ) in the treatment of patients with this disease has been a major focus of discussion on the news and social media. Despite the lack of good data supporting its use in the clinical setting, there have been numerous reports of individual consumption of HCQ resulting in accidental overdose and even death. It is therefore important to recognize and manage patients who may present with HCQ toxicity.
As the COVID-19 pandemic continues to unravel, the role of hydroxychloroquine (HCQ) in the treatment of patients with this disease has been a major focus of discussion on the news and social media. Despite the lack of good data supporting its use in the clinical setting, there have been numerous reports of individual consumption of HCQ resulting in accidental overdose and even death. It is therefore important to recognize and manage patients who may present with HCQ toxicity.
 A 35-year-old female emergency medicine physician presents for evaluation for severe myalgias, headache, fatigue, mild nasal congestion, profound anosmia, cough, and subjective fevers and chills. She has no measured temperature above 100.4°F, but has been taking anti-inflammatories around the clock. The day previously, she called occupational health and received testing for the novel coronavirus. The next day, her test returns positive. What happens next? We are here to share our personal experiences with COVID-19 and provide some resources to best support yourselves, your families, your learners, and your colleagues throughout this uncertain and ever-changing situation.
A 35-year-old female emergency medicine physician presents for evaluation for severe myalgias, headache, fatigue, mild nasal congestion, profound anosmia, cough, and subjective fevers and chills. She has no measured temperature above 100.4°F, but has been taking anti-inflammatories around the clock. The day previously, she called occupational health and received testing for the novel coronavirus. The next day, her test returns positive. What happens next? We are here to share our personal experiences with COVID-19 and provide some resources to best support yourselves, your families, your learners, and your colleagues throughout this uncertain and ever-changing situation.