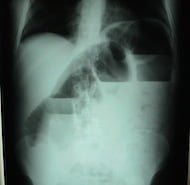
Ultrasound For The Win! – 46M with Diffuse Abdominal Pain #US4TW
Welcome to another ultrasound-based case, part of the “Ultrasound For The Win!” (#US4TW) Case Series. In this case series, we focus on a real clinical case where point-of-care ultrasound changed the management of a patient’s care or aided in the diagnosis. In this case, a 46-year-old man with a history of alcohol abuse presents with diffuse abdominal pain.
(more…)


 Your triage nurse complains of numerous patients in the waiting room complaining of nausea, retching, and emesis. They ask you “why can’t we have an antiemetic on hand in triage?” Turns out they might have had an effective antiemetic on hand, or rather in their scrub pocket the entire time. They just didn’t know about it yet.
Your triage nurse complains of numerous patients in the waiting room complaining of nausea, retching, and emesis. They ask you “why can’t we have an antiemetic on hand in triage?” Turns out they might have had an effective antiemetic on hand, or rather in their scrub pocket the entire time. They just didn’t know about it yet. Recall the last time you were sitting in a room doing a large-volume, therapeutic paracentesis in the ED. Were you stressing out because your other patients were still being actively managed? Large-volume paracentesis is a common and important part of our practice, but often requires your dedicated time at the bedside. Additionally, what do you do if you do not have the fancy paracentesis kit or vacuum collection bottles?
Recall the last time you were sitting in a room doing a large-volume, therapeutic paracentesis in the ED. Were you stressing out because your other patients were still being actively managed? Large-volume paracentesis is a common and important part of our practice, but often requires your dedicated time at the bedside. Additionally, what do you do if you do not have the fancy paracentesis kit or vacuum collection bottles?