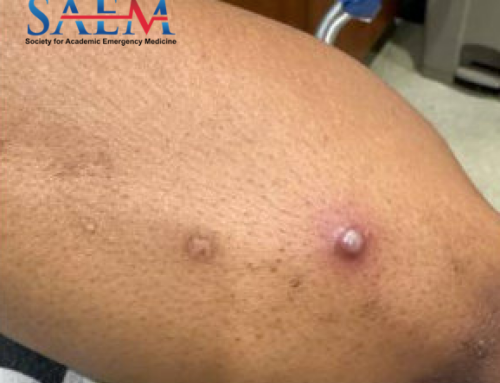
A 37-year-old female presented to the emergency department for evaluation of numbness and discoloration to her left fourth finger, which had started the day before. The patient stated that she was gardening the previous day and afterward she noticed the discoloration and pain. The patient denied taking any medications. She reported recreational methamphetamine and heroin use. She denied any chest pain or difficulty breathing. She denied any history of Raynaud’s phenomenon, venous thromboembolism, or history of trauma. The patient was afebrile with normal vital signs. Physical exam revealed cyanotic discoloration to the left distal fourth finger. Sensation was intact to light touch and strength was 5 out of 5 in the finger. The capillary refill was diminished. Radial and ulnar pulses were 2+ bilaterally. Initially, a warm pack was placed to the patient’s finger with slight improvement, but without resolution of the pain and cyanosis. What is the diagnosis?
A 37-year-old female presented to the emergency department for evaluation of numbness and discoloration to her left fourth finger, which had started the day before. The patient stated that she was gardening the previous day and afterward she noticed the discoloration and pain. The patient denied taking any medications. She reported recreational methamphetamine and heroin use. She denied any chest pain or difficulty breathing. She denied any history of Raynaud’s phenomenon, venous thromboembolism, or history of trauma. The patient was afebrile with normal vital signs. Physical exam revealed cyanotic discoloration to the left distal fourth finger. Sensation was intact to light touch and strength was 5 out of 5 in the finger. The capillary refill was diminished. Radial and ulnar pulses were 2+ bilaterally. Initially, a warm pack was placed to the patient’s finger with slight improvement, but without resolution of the pain and cyanosis. What is the diagnosis?
Septic Embolism from Mitral Valve Endocarditis
Explanation:
Endocarditis is the inflammation of the endocardium, often caused by infection [1]. Endocarditis is associated with high morbidity and mortality and remains a serious health problem worldwide. In hospitalized patients, mortality is still near 20% [2]. The incidence of endocarditis in the United States is approximately 15,000 cases per year [3]. Risk factors include [1]:
- structural heart disease
- invasive medical procedures
- presence of a mechanical valve
- injection drug use
Endocardial injury can lead to the formation of vegetations, which can become seeded with bacteria. Important considerations [1]:
- Embolic events occur in 20-50% of patients.
- The highest percent of embolization occurs to the central nervous system followed by the gastrointestinal tract, kidneys, and lungs.
- Larger vegetations are more likely to embolize.
Management priorities include stabilization of the patient and initiation of antibiotics in all cases. Blood cultures should be obtained every 24-48 hours until they are negative. The risk of embolization decreases once antimicrobial treatment is started [1]. Septic emboli should be considered in patients presenting with risk factors for endocarditis and otherwise unexplained embolic events.
Case Conclusion
Vascular surgery was consulted; they recommended a trial of nitroglycerin ointment and a CT angiogram of the left upper extremity. CT angiogram was obtained of the upper extremity which did not show any large vessel occlusion. However, the fourth finger inter-digitalis lacked opacification. Given concern for an embolic event leading to the patient’s findings, an echocardiogram was obtained which showed a large multilobular echo dense mass measuring 2.5 x 2 cm attached to the atrial surface of the anterior mitral leaflet. This was suggestive of vegetation. Blood cultures were obtained and the patient was started on vancomycin and cefepime for treatment of suspected endocarditis. MRI of the brain showed multiple peripheral punctate left frontal-parietal lesions suggestive of acute embolic infarcts. The patient completed six weeks of intravenous antibiotics with a plan for outpatient cardiology follow up.
References
Check out the Diagnose on Sight archives
- McDonald JR. Acute infective endocarditis. Infect Dis Clin North Am. 2009;23(3):643–664. PMID: 19665088
- Yang, A., et al. Clinical and echocardiographic predictors of embolism in infective endocarditis: systematic review and meta-analysis. Clinical Microbiology and Infection. 2019; 25.2:178-187. PMID: 30145401
- Slipczuk, Leandro, et al. Infective endocarditis epidemiology over five decades: a systematic review. PloS one. 2013; 8.12. PMID: 24349331