Trick of the Trade: "Pour some sugar on me" | Reducing a rectal prolapse
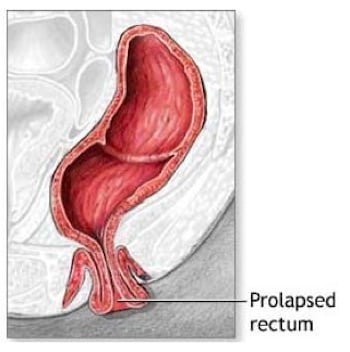 Rectal prolapses are typically caused by weakened rectal muscles, continued straining, stresses during childbirth, weakened ligaments, or neurological deficits.
Rectal prolapses are typically caused by weakened rectal muscles, continued straining, stresses during childbirth, weakened ligaments, or neurological deficits.
How do you fix them? You can attempt manual reduction of the prolapse by using direct pressure. On the other extreme, corrective surgery can be performed from either an abdominal or perineal approach.
Trick of the Trade: Pour some sugar on it.
Def Leppard may have been right. Rectal prolapses often are associated with quite a bit of rectal mucosal edema. Sprinkle granulated sugar onto the area. Wait 15 minutes. The sugar reduces the edema by osmotically drawing out the fluid. The prolapse often reduces spontaneously or with gentle manual pressure.
References
- Ramanujam PS, Venkatesh KS. Management of acute incarcerated rectal prolapse. Dis Colon Rectum. Dec 1992;35(12):1154-6.
- Coburn WM III, Russell MA, Hofstetter WL. Sucrose as an aid to manual reduction of incarcerated rectal prolapse. Ann Emerg Med. Sep 1997;30(3):347-9.

 Anyone who teaches medicine asks students to list their differential diagnosis when discussing a new clinical case. It’s also part of several models for education including the One-Minute Preceptor and SNAPPS.
Anyone who teaches medicine asks students to list their differential diagnosis when discussing a new clinical case. It’s also part of several models for education including the One-Minute Preceptor and SNAPPS.



