SplintER Series: Funny Looking Finger

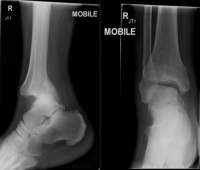
Figure 1: Terminal extensor tendon avulsion at distal interphalangeal joint of 5th digit
A 17-year-old baseball player presents complaining of finger pain and difficulty straightening his finger after a baseball game. You obtain x-rays and see the following fracture (photo credit).
What is your diagnosis and emergency department management?




 A 32 year old woman arrives in your emergency department after being in a motor vehicle collision where she was the seat-belted driver. She undergoes chest CT imaging despite a negative chest x-ray because of her ongoing anterior chest wall diffuse tenderness. You discover a small 10% pneumothorax (PTX), but no other associated thoracic injuries. Should you place a tube thoracostomy (chest tube)? Should this patient be admitted to the hospital? A 2019 Annals of Emergency Medicine paper by the NEXUS Chest research group tackles these questions.
A 32 year old woman arrives in your emergency department after being in a motor vehicle collision where she was the seat-belted driver. She undergoes chest CT imaging despite a negative chest x-ray because of her ongoing anterior chest wall diffuse tenderness. You discover a small 10% pneumothorax (PTX), but no other associated thoracic injuries. Should you place a tube thoracostomy (chest tube)? Should this patient be admitted to the hospital? A 2019 Annals of Emergency Medicine paper by the NEXUS Chest research group tackles these questions. Welcome to Leg Day #2 of the
Welcome to Leg Day #2 of the