Pediatric Emergency Medicine (PEM) Pearls
Created in 2015, this series is hosted by Dr. Jessica Chow and Dr. Josh Bukowski who are authors and editors for this series which focuses on evidence-based care in the realm of pediatric emergency medicine.
 Regional nerve blocks of the face and ear can be a wonderful choice of analgesia in a child, particularly for wounds that need to be repaired. The benefits include fewer local injections, improved cosmesis due to less wound margin distortion, and improved analgesia within the nerve region.1,2 The following blog post and brief video tutorial review the key elements of this technique.
Regional nerve blocks of the face and ear can be a wonderful choice of analgesia in a child, particularly for wounds that need to be repaired. The benefits include fewer local injections, improved cosmesis due to less wound margin distortion, and improved analgesia within the nerve region.1,2 The following blog post and brief video tutorial review the key elements of this technique.
 The standard for diagnosing pneumonia is a combination of the clinical history, physical examination, and chest x-ray (CXR) findings. However, lung ultrasound (US) has been shown to be a reasonable alternative to CXR in children, and may be an appropriate alternative diagnostic imaging modality in the Emergency Department (ED).
The standard for diagnosing pneumonia is a combination of the clinical history, physical examination, and chest x-ray (CXR) findings. However, lung ultrasound (US) has been shown to be a reasonable alternative to CXR in children, and may be an appropriate alternative diagnostic imaging modality in the Emergency Department (ED).
 A 3 year-old boy presents with a deep laceration of the distal phalanx, through the nail bed, after slamming his fingers in a car door. He is crying, anxious, and uncooperative. How do you make this situation easier to evaluate and repair?
A 3 year-old boy presents with a deep laceration of the distal phalanx, through the nail bed, after slamming his fingers in a car door. He is crying, anxious, and uncooperative. How do you make this situation easier to evaluate and repair?
Nail bed and finger laceration repairs can be challenging, and even more challenging in young patients. Preparation is key to getting a good outcome. Here we present a pediatric trick of the trade on immobilizing a finger for digit or nail bed procedures.
 Insulin does MANY things in the body, but the role we care about in the Emergency Department is glucose regulation. Insulin allows cells to take up glucose from the blood stream, inhibits liver glucose production, increases glycogen storage, and increases lipid production. When insulin is not present, such as in patients with Type 1 diabetes mellitus (DM), all of the opposite effects occur.
Insulin does MANY things in the body, but the role we care about in the Emergency Department is glucose regulation. Insulin allows cells to take up glucose from the blood stream, inhibits liver glucose production, increases glycogen storage, and increases lipid production. When insulin is not present, such as in patients with Type 1 diabetes mellitus (DM), all of the opposite effects occur.
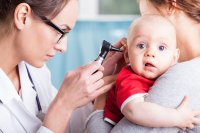 While ear foreign bodies can happen at any age, the majority occur in children less than 7 years of age.1 The younger the patient, the less likely they are cooperative with the exam and, therefore, the less chance of successful foreign body removal. The first attempt at removal is the best, so it is important to make it count. Similarly, different types of foreign bodies call for different “tools” for removal. It is important to understand when to attempt removal in the emergency department (ED) and what tools are available. This blog post will help you optimize your first pass success at foreign body removal by understanding what tools are at your disposal.
While ear foreign bodies can happen at any age, the majority occur in children less than 7 years of age.1 The younger the patient, the less likely they are cooperative with the exam and, therefore, the less chance of successful foreign body removal. The first attempt at removal is the best, so it is important to make it count. Similarly, different types of foreign bodies call for different “tools” for removal. It is important to understand when to attempt removal in the emergency department (ED) and what tools are available. This blog post will help you optimize your first pass success at foreign body removal by understanding what tools are at your disposal.
 Pediatric community-acquired pneumonia (CAP) is an acute, common, and potentially serious infection of the pulmonary parenchyma in children. In November 2010, the American Academy of Pediatrics endorsed “The management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America.” [PDF]1Based on this guideline, the American Academy of Pediatrics (AAP) Section on Emergency Medicine’s Committee on Quality Transformation developed a clinical algorithm for CAP in the ED setting.
Pediatric community-acquired pneumonia (CAP) is an acute, common, and potentially serious infection of the pulmonary parenchyma in children. In November 2010, the American Academy of Pediatrics endorsed “The management of community-acquired pneumonia in infants and children older than 3 months of age: clinical practice guidelines by the Pediatric Infectious Diseases Society and the Infectious Diseases Society of America.” [PDF]1Based on this guideline, the American Academy of Pediatrics (AAP) Section on Emergency Medicine’s Committee on Quality Transformation developed a clinical algorithm for CAP in the ED setting.
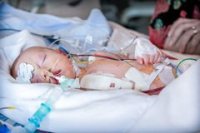 Just as in adults, pediatric sepsis is a complex topic with continued research. In the United States, there are an estimated 75,000 cases per year of pediatric severe sepsis with an in-hospital mortality of 5-10%.1,2 This is one of the deadliest conditions treated in children. In addition, after the Rory Staunton case, New York State passed regulations requiring all hospitals to have pediatric specific recognition, treatment, and data reporting systems. Several other states have adopted, or are considering, similar requirements. Thus it is critical that emergency physicians understand at least the basics of pediatric sepsis management.
Just as in adults, pediatric sepsis is a complex topic with continued research. In the United States, there are an estimated 75,000 cases per year of pediatric severe sepsis with an in-hospital mortality of 5-10%.1,2 This is one of the deadliest conditions treated in children. In addition, after the Rory Staunton case, New York State passed regulations requiring all hospitals to have pediatric specific recognition, treatment, and data reporting systems. Several other states have adopted, or are considering, similar requirements. Thus it is critical that emergency physicians understand at least the basics of pediatric sepsis management.