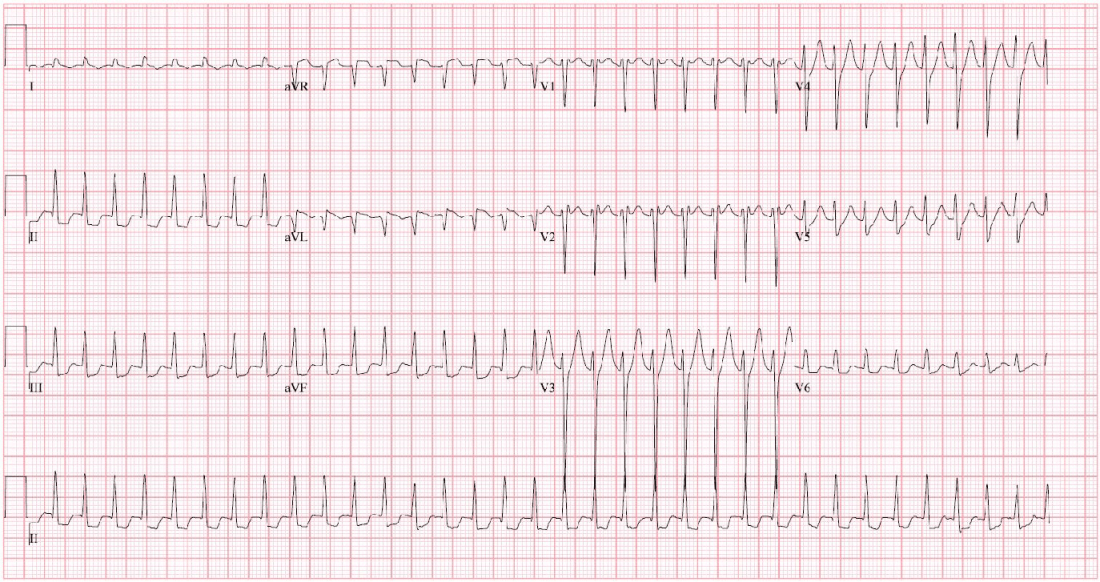
SAEM Clinical Image Series: A Young Woman with Chest Pain
A 35-year-old female with a history of intermittent palpitations who is three months post-partum presented to the emergency department (ED) with three days of sharp, substernal chest pain radiating down her left arm. She reportedly had a normal electrocardiogram (ECG) at an outside hospital on the first day of symptoms. The pain returned and was associated with one episode of vomiting the night prior to presenting to our ED. Initial ECG on arrival is shown. Vitals: Tachycardic; afebrile; normotensive; no tachypnea or hypoxemia on room air General: Mild distress, appears uncomfortable Cardiovascular: Tachycardic to 100s, regular rhythm, no murmur, normal peripheral perfusion, no edema Pulmonary: Lungs clear to auscultation, no respiratory distress Neuro: Alert and oriented, neurologically intact Complete blood count (CBC) and basic metabolic panel (BMP): unremarkable Partial thromboplastin time (PTT) and international normalized ratio (INR): normal Troponin: 42 Spontaneous coronary artery dissection (SCAD). The patient underwent emergent coronary angiography demonstrating multivessel coronary dissection including a distal left anterior descending (LAD) hematoma with lumen compression as well as obtuse marginal (OM1) and posterior descending artery (PDA) lesions consistent with spontaneous coronary artery dissection (SCAD). She was admitted to the intensive care unit on a heparin drip, had decreasing troponin levels, and ultimately was discharged home on enalapril, metoprolol, aspirin, and clopidogrel. SCAD is a rare but important diagnosis in the ED as it conveys serious morbidity and mortality risk. Patients present with chest pain, dyspnea, diaphoresis, and potentially signs or symptoms of heart failure from severe ischemia. Most patients are women under the age of 50, and many are pregnant, postpartum, or taking oral contraceptives. This may be mistaken for other diagnoses on presentation, such as ST-segment elevation myocardial infarction (STEMI) or takotsubo cardiomyopathy, which usually presents in post-menopausal patients, but SCAD differs in its typical patient population. Wall motion abnormalities on an echocardiogram are present, but there are not always signs of heart failure as in post-partum cardiomyopathy. Patients are often taken for urgent coronary angioplasty, though in cases with marked ischemia or hemodynamic instability, emergent coronary artery bypass graft (CABG) may be indicated. Recurrence is common; patients should be counseled on mitigating cardiovascular risk factors, particularly smoking and hypertension, and to be cautious with intense exertion and future pregnancies. Sex, age, and postpartum status. Images and cases from the Society of Academic Emergency Medicine (SAEM) Clinical Images Exhibit at the 2021 SAEM Annual Meeting | Copyrighted by SAEM 2021 – all rights reserved. View other cases from this Clinical Image Series on ALiEM.
Take-Home Points
Copyright