Diagnose on Sight: Case of a red, swollen neck
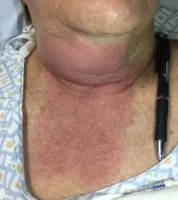 Case: A 78 year-old female with a past medical history of asthma and hypothyroidism presents with a three day history of sore throat and a two day history of a “lump” along the right side of her neck. The “lump” has now progressed to involve both sides of her anterior neck and is accompanied with erythema, tenderness to palpation, and swelling. In addition, the patient has developed a hoarse voice and odynophagia. The patient’s primary care physician referred her to an ENT specialist, who then referred the patient to the ED for urgent imaging due to the concern for a deep space neck infection. Triage vitals are remarkable for a heart rate of 118 beats per minute. She is otherwise normotensive and afebrile. On physical exam, slight crepitation in noted on the floor of the patient’s mouth. Of note, the patient also informs you of her penicillin allergy. Which of the following is the biggest risk factor for this particular disease process?
Case: A 78 year-old female with a past medical history of asthma and hypothyroidism presents with a three day history of sore throat and a two day history of a “lump” along the right side of her neck. The “lump” has now progressed to involve both sides of her anterior neck and is accompanied with erythema, tenderness to palpation, and swelling. In addition, the patient has developed a hoarse voice and odynophagia. The patient’s primary care physician referred her to an ENT specialist, who then referred the patient to the ED for urgent imaging due to the concern for a deep space neck infection. Triage vitals are remarkable for a heart rate of 118 beats per minute. She is otherwise normotensive and afebrile. On physical exam, slight crepitation in noted on the floor of the patient’s mouth. Of note, the patient also informs you of her penicillin allergy. Which of the following is the biggest risk factor for this particular disease process?





