Trick of the Trade: Speed up ECG paper rate to differentiate tachycardias
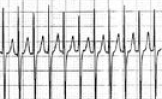
Undifferentiated tachycardias, especially when the rate is extremely fast, make it difficult to see anything other than the QRS complexes! Is there a P or flutter wave?
(more…)






 A 50 y/o man with a history of CHF and COPD is brought in by ambulance in severe respiratory distress. He is sitting upright with a RR 30 and O2 saturation of 79% on room air. Is this a CHF or COPD exacerbation? This is a common dilemma faced in the ED. Fortunately there are likelihood ratios to help you risk stratify using a Fagan nomogram.
A 50 y/o man with a history of CHF and COPD is brought in by ambulance in severe respiratory distress. He is sitting upright with a RR 30 and O2 saturation of 79% on room air. Is this a CHF or COPD exacerbation? This is a common dilemma faced in the ED. Fortunately there are likelihood ratios to help you risk stratify using a Fagan nomogram.