Trick of the Trade: Laryngospasm notch maneuver
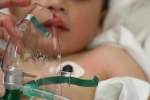 What is the incidence of laryngospasm in pediatric patients receiving ketamine for procedural sedation in the ED?
What is the incidence of laryngospasm in pediatric patients receiving ketamine for procedural sedation in the ED?
A child with laryngospasm can be a scary thing to manage. There’s no way to predict whether a child is going to get it.
You can try the usual maneuvers including a jaw-thrust, positive pressure ventilation to try to open the vocal cords, and suctioning. If these don’t work, you might consider giving the patient a paralytic, such as succinylcholine, and performing an endotracheal intubation for worsening hypoxia. Before that, what non-invasive maneuver can you try first?



 Ingrown toenails, or paronychias, are usually exquisitely painful and a bit gnarly when they present to you in the Emergency Department. Dr. Stella Yiu described toenail splinting techniques using steristrips or dental floss. The purpose of splinting is to prevent the toenail from growing back into the lateral nail fold.
Ingrown toenails, or paronychias, are usually exquisitely painful and a bit gnarly when they present to you in the Emergency Department. Dr. Stella Yiu described toenail splinting techniques using steristrips or dental floss. The purpose of splinting is to prevent the toenail from growing back into the lateral nail fold.