Atraumatic Low Back Pain: ACEP E-QUAL Network Podcast
 Atraumatic low back pain is a common complaint in the ED. For most patients, a thorough history and physical exam is sufficient to exonerate causes that threaten life or neurological function. For a small subset, however, MRI may be required. ALiEM has partnered with the ACEP E-QUAL Network to promote clinical practice improvements through a series of podcasts. In our first installment, we focus on this common presentation. We review highlights from an interview with Dr. Jonathan Edlow, Vice Chair of Emergency Medicine at Beth Israel Deaconess, about the presentation and evaluation of low back pain. Afterward be sure to check out the podcast in full.
Atraumatic low back pain is a common complaint in the ED. For most patients, a thorough history and physical exam is sufficient to exonerate causes that threaten life or neurological function. For a small subset, however, MRI may be required. ALiEM has partnered with the ACEP E-QUAL Network to promote clinical practice improvements through a series of podcasts. In our first installment, we focus on this common presentation. We review highlights from an interview with Dr. Jonathan Edlow, Vice Chair of Emergency Medicine at Beth Israel Deaconess, about the presentation and evaluation of low back pain. Afterward be sure to check out the podcast in full.
(more…)



 A young man is brought into an emergency department after an electric lawn edger cut through his work boot and into the dorsum of his right foot. He has a clearly contaminated 5 cm x 1 cm laceration on the lateral side, and an underlying tendon is exposed. Sensation is diminished around the wound and he is unable to actively extend his 5th toe past a neutral position. How would you diagnose and repair his extensor tendon injury?
A young man is brought into an emergency department after an electric lawn edger cut through his work boot and into the dorsum of his right foot. He has a clearly contaminated 5 cm x 1 cm laceration on the lateral side, and an underlying tendon is exposed. Sensation is diminished around the wound and he is unable to actively extend his 5th toe past a neutral position. How would you diagnose and repair his extensor tendon injury?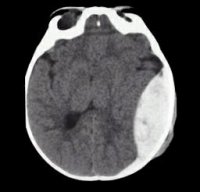 Robust and comprehensive studies now support specific management guidelines for patients presenting with different intracranial hemorrhages (ICH). From the Emergency Department perspective, the primary dilemmas involve specific blood pressure goals and whether seizure prophylaxis with phenytoin is necessary. The
Robust and comprehensive studies now support specific management guidelines for patients presenting with different intracranial hemorrhages (ICH). From the Emergency Department perspective, the primary dilemmas involve specific blood pressure goals and whether seizure prophylaxis with phenytoin is necessary. The